Last Updated: April 2026
This article is reviewed periodically to reflect current dermatology information and treatment approaches.
WARNING: Some images may be slightly graphic in nature due to the conditions described.
Jock itch, ringworm, yeast infection, chafing — they all show up in the same place, they all itch, and they all look vaguely similar when you’re stressed and staring at a rash. Here’s how to actually tell them apart.
The distinction matters because the care is different. Antifungal treatment addresses a fungal infection. A skin repair ointment handles friction damage. A yeast infection responds to a different antifungal approach than jock itch does. Getting it wrong doesn’t just waste time — it can occasionally make things worse. So a few minutes spent reading this is worth it.
At a Glance
Jock itch, ringworm, and yeast infections can look similar—but differ in cause, appearance, and treatment, which is why accurate identification is critical for effective care.
All five conditions covered in this guide can cause itching and redness in the groin area — but they have meaningfully different causes, appearances, and care approaches:
- Jock itch (tinea cruris) — a fungal infection; ring-shaped, dry, scaly rash with a defined border; contagious
- Ringworm (tinea corporis) — same family of fungus as jock itch; circular rash with a clearer center; appears on the body
- Yeast infection (candidal intertrigo) — caused by Candida yeast; bright red, wet-looking rash; often has small satellite pustules at the edges
- Balanitis — inflammation of the head of the penis; caused by yeast, bacteria, or irritation; redness, swelling, and sometimes discharge — men only
- Chafing — not an infection at all; caused purely by friction; raw, stinging, no defined border, no advancing edge
- Herpes (genital HSV) — a viral infection; painful, fluid-filled blisters that crust over; recurs in outbreaks
Key Takeaways
- Jock itch and ringworm are caused by the same type of fungus — location on the body is what distinguishes them
- A yeast infection looks wetter and redder than a fungal tinea rash — and it often behaves differently too
- Balanitis affects the head of the penis specifically — it’s a different condition from jock itch, even though both involve the groin area
- Chafing has no defined border and improves with rest and friction reduction — a fungal rash won’t do either of those things
- Herpes causes painful blisters that crust over — jock itch causes an itchy rash, not painful sores
- When something doesn’t add up or isn’t improving, a healthcare provider can confirm what’s going on quickly
Our commitment to accurate, evidence-based information: This article draws on peer-reviewed research and trusted health organizations including the Cleveland Clinic, Merck Manual, Harvard Health Publishing, StatPearls/NCBI, DermNet NZ, and the CDC. All sources are numbered and linked in the references section below.
The Full Comparison at a Glance
Before we go into each condition in depth, here’s a side-by-side overview. You can use this as a quick reference, or come back to it after reading each section once you have a better sense of what you’re looking for.
Feature | Jock Itch | Ringworm | Yeast Infection | Balanitis | Chafing | Herpes |
|---|---|---|---|---|---|---|
Cause | Dermatophyte fungus (tinea) | Dermatophyte fungus (tinea) | Candida yeast overgrowth | Candida yeast, bacteria, or skin irritation | Friction — skin on skin or fabric | Herpes simplex virus (HSV-1 or HSV-2) |
Appearance | Red, ring-shaped, scaly with a defined raised border | Circular rash, raised border, center clears as it spreads | Bright red, moist, “beefy” — satellite pustules at edges | Redness, swelling, shiny or white patches on the head of the penis — may have discharge | Red, raw, uniform — no distinct edge or border | Clusters of small fluid-filled blisters that break and crust over |
Texture | Dry, flaky, scaly | Dry, scaly, raised ring edge | Moist, shiny, may weep slightly | Shiny, swollen, sometimes glazed-looking skin on glans | Raw, hot to the touch | Wet blisters, then painful crusted sores |
Location | Groin crease, inner thighs, buttocks — usually spares the scrotum | Anywhere on the body: arms, legs, torso | Skin folds, groin — often involves scrotum or vulva | Head (glans) of the penis and foreskin only — men only | Inner thighs, groin, any area with repeated friction | Genitals, thighs, buttocks, around the anus |
Main sensation | Intense itching, sometimes burning | Itching, occasionally mild burning | Burning, itching, soreness — often rawer than jock itch | Itching, tenderness, burning — pain during urination in some cases | Stinging, raw, hot — more painful than itchy | Pain and tenderness, tingling before blisters appear |
Contagious? | Yes — skin contact, shared towels or clothing | Yes — skin contact, contaminated surfaces | Not in the same way as tinea | Can transfer between partners when caused by yeast | No | Yes — primarily through sexual or close skin contact |
Worsened by | Heat, sweat, tight clothing | Heat, moisture, prolonged skin contact | Antibiotic use, heat, moisture, high blood sugar | Poor hygiene under foreskin, diabetes, tight foreskin | Physical activity, moisture, repetitive movement | Stress, illness, immune system changes |
Prevention | Keep area dry, breathable underwear, socks before underwear, treat athlete’s foot | Keep area dry, avoid sharing towels or clothing, treat athlete’s foot | Keep area dry, breathable underwear, change promptly after sweating, mindful after antibiotics | Clean under foreskin daily, keep area dry, manage blood sugar, use gentle cleansing products | Breathable fabrics, moisture-wicking clothing, reduce friction sources, dry skin thoroughly | Avoid sharing towels or clothing, practice safe sex, regular STI screening |
Treatment |
What Is Jock Itch?
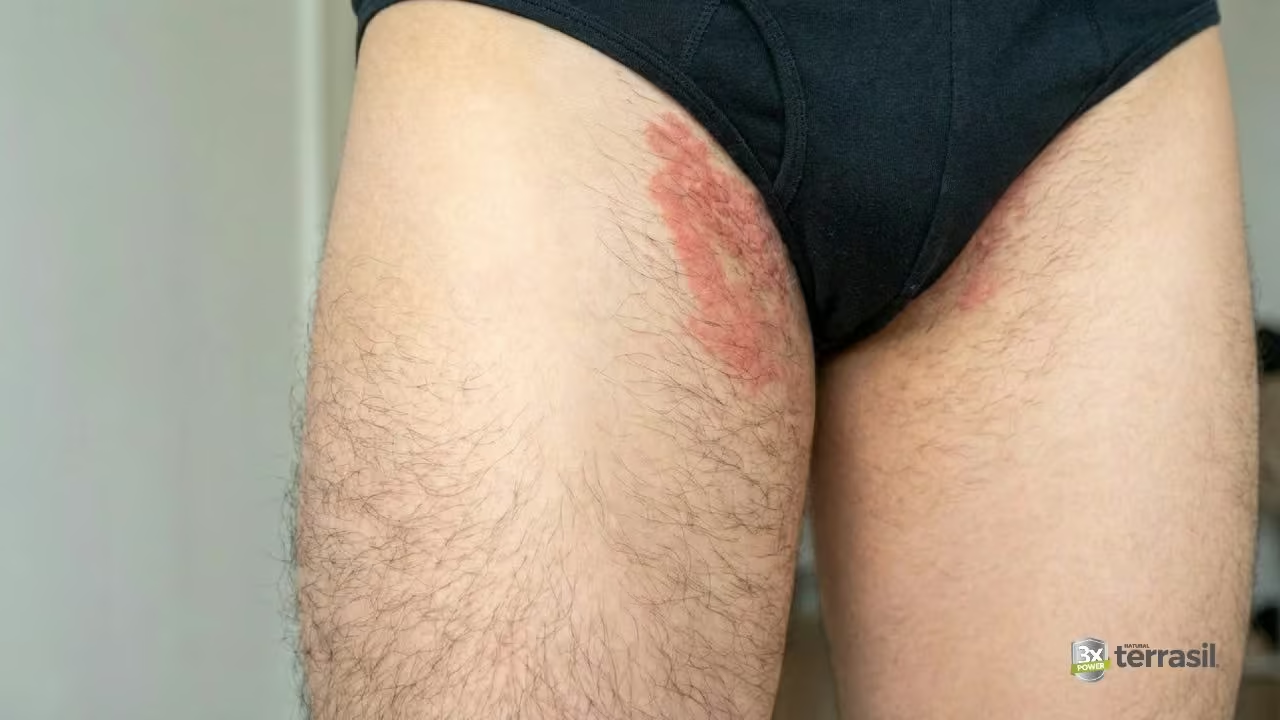
Jock itch — medically known as tinea cruris — is a fungal skin infection that develops in the groin area. The “jock” part of the name is a bit misleading, because you absolutely don’t need to be an athlete to get it. Anyone who sweats regularly, wears tight clothing, or spends time in warm and humid conditions can develop jock itch. It’s more common than most people realize, and it’s nothing to be embarrassed about.1
The cause is a group of fungi called dermatophytes — the same organisms responsible for athlete’s foot and ringworm. In fact, jock itch is technically a form of ringworm: tinea in the groin. Dermatophytes thrive in warm, moist, dark environments, which makes the groin a near-ideal location for them to grow, especially when clothing traps heat and sweat against the skin.2
Men tend to develop jock itch more often than women, largely because moisture can get trapped between the scrotum and the inner thigh. People with diabetes, obesity, or a weakened immune system are also at higher risk, because their skin folds may stay damp for extended periods.3
What jock itch actually looks like
The rash typically starts near the crease of the groin, high on the inner thigh, and slowly spreads outward. As it does, it often takes on a ring-like or half-moon shape — the outer edges are redder, raised, scaly, and more active, while the center of the rash may partially clear. That defined, advancing border is one of the most reliable signs that you’re looking at a fungal infection rather than something else.4
It itches — often intensely. Physical activity tends to make it worse because sweat and heat feed the fungus. The scrotum is usually spared or only mildly involved, which is a useful detail when comparing jock itch to a yeast infection. The rash is predominantly dry and flaky rather than wet or shiny.5
How it spreads — including to yourself
Jock itch is contagious. It can spread through direct skin contact or through shared towels, underwear, or clothing. One route that catches people off guard: the fungus can travel from an active athlete’s foot infection to the groin through clothing when you get dressed. Pulling underwear over feet that carry the fungus is enough to transfer it. Putting socks on before underwear is a simple habit that breaks that cycle.1
TERRASIL® Jock Itch Treatment MAX is formulated with clotrimazole, an FDA-recognized antifungal ingredient, combined with patented Activated Minerals® technology to support skin comfort during the clearing process. For a more complete approach, the Serious Jock Itch Cure 2-Product System pairs the ointment with an antifungal cleansing step.
What Is Ringworm — and Is It the Same as Jock Itch?

This is one of the most common questions people have, and the answer might surprise you: they’re caused by exactly the same type of fungus. Ringworm (tinea corporis) and jock itch (tinea cruris) are both dermatophyte infections — the only real difference is where on the body they appear. Ringworm is the name used when tinea shows up on the arms, legs, torso, or trunk. Jock itch is the same infection in the groin. If you want a deeper breakdown of treatment options, see what actually works for ringworm treatment.
And just to clear something up: ringworm has nothing to do with worms. The name comes from the shape the rash tends to form — a ring. That’s it. Entirely a fungal infection.6
What ringworm looks like
The classic ringworm rash is circular or oval, with a raised, scaly, reddish border and a center that looks relatively clear or less inflamed. The outer ring is where the active fungal growth is happening — it’s redder, slightly elevated, and may feel rough. Over time, the ring may expand outward while the center continues to flatten and clear, making that ring shape increasingly distinct.6
It’s itchy, occasionally accompanied by a mild burning sensation, and it can appear virtually anywhere on the body. That flexibility in location is what separates it from jock itch in practical terms.
Can you use jock itch treatment for ringworm?
Yes — because they’re caused by the same fungus, antifungal ingredients that address jock itch work through the same mechanism against ringworm. Clotrimazole, for example, disrupts the fungal cell membrane regardless of which part of the body the infection has settled on.7
TERRASIL® Ringworm Treatment MAX Ointment combines clotrimazole with Activated Minerals® and botanical ingredients formulated to support skin comfort during recovery from tinea infections on the body. TERRASIL® Antifungal Treatment MAX is a broader option that may also be relevant for both jock itch and ringworm depending on the situation.
What Is a Groin Yeast Infection?

A groin yeast infection is caused by a completely different organism than jock itch — Candida, most commonly Candida albicans. This yeast naturally lives on the skin in small amounts without causing any problems. Under certain conditions, though, it can overgrow and trigger an infection. When that happens in the skin folds, the condition is called candidal intertrigo.8
It’s worth knowing what conditions tend to set the stage for this. Recent antibiotic use is a big one — antibiotics disrupt the natural balance of bacteria and yeast on the skin, and Candida takes advantage. Diabetes, obesity, a weakened immune system, and prolonged exposure to heat and moisture are also common contributing factors.9 If you’ve recently finished a round of antibiotics and now have a groin rash, that context matters.
What a groin yeast infection looks like — and how it differs from jock itch
This is where the distinction becomes most useful. A candidal rash looks different from jock itch in ways you can actually see. It tends to appear brighter red — more intensely colored, sometimes described as “beefy” — and it looks wet rather than dry. Where jock itch is scaly and flaky, a yeast rash is more shiny and moist, and may even weep slightly. One of the most characteristic features is the presence of satellite pustules: small red bumps that appear just beyond the main rash border, scattered outward like satellites around a central mass.10
Unlike jock itch, which typically spares the scrotum, a candidal infection more often involves the scrotum directly. In women, it commonly affects the vulva and surrounding skin. The sensation tends to feel more raw and burning than the deep, persistent itch of jock itch.8
A quick pattern to remember: Dry and scaly with a ring border pointing toward jock itch (fungal tinea). Wet, intensely red, with satellite pustules pointing toward yeast (Candida). These two are frequently confused, and they respond to different types of care — so the distinction is worth making.
For external intimate skin discomfort, FEMMESIL® Cream and FEMMESIL® Ultra Therapy Ointment are formulated with sensitive intimate skin in mind. The FEMMESIL® Ultra Therapy Vaginal Ointment & Cleansing Bar Kit pairs a cleansing step with topical care for a more complete routine.
Can Men Get a Yeast Infection? Can Women Get Jock Itch?

Yes to both — and this is genuinely one of the most underappreciated points when it comes to groin rashes. These conditions are not gender-exclusive, even though they’re often talked about as if they are.
Men and yeast infections
Men can absolutely develop a groin yeast infection, and it’s more common than most people realize. Candida yeast lives naturally on everyone’s skin — it doesn’t discriminate. When the conditions are right (heat, moisture, antibiotic use, high blood sugar, or a disrupted skin barrier), it can overgrow on male skin just as it does elsewhere.9
In men, a candidal groin infection often presents as a bright red, moist rash that involves the scrotum — which is one of the clearest ways to distinguish it from jock itch, since jock itch typically spares the scrotum. The rash may have that characteristic “beefy” appearance, and small satellite pustules scattered just beyond the rash border are another telling sign that Candida is involved rather than a dermatophyte fungus.10
Men with diabetes are particularly susceptible, as elevated blood sugar creates favorable conditions for yeast overgrowth. Recent antibiotic use is another common trigger. If a groin rash appears shortly after finishing antibiotics, a yeast infection is worth considering — even in men who’ve never had one before.
Women and jock itch
Jock itch is far more common in men, but women do get it — and the same fungus is responsible. Trichophyton rubrum, the dermatophyte most often associated with tinea cruris, doesn’t distinguish between genders. Women who sweat heavily, wear tight synthetic clothing during exercise, or have athlete’s foot are all at risk of developing jock itch in the groin or inner thigh.5
The rash looks the same in women as it does in men: a red, scaly, ring-shaped rash with a defined border that spreads outward from the groin crease. It tends to affect the upper inner thighs and the skin folds around the groin rather than the genitals directly. Because women are less commonly diagnosed with jock itch, it sometimes goes misidentified as a yeast infection — but the two look meaningfully different once you know what to look for.
The key takeaway: If you’re a man with a bright red, wet-looking rash that involves the scrotum — don’t automatically assume jock itch. If you’re a woman with a dry, scaly, ring-shaped rash on the inner thigh — don’t automatically assume it isn’t jock itch. The appearance tells you more than the gender does.
For women dealing with external intimate skin discomfort — whether from a yeast infection or general irritation — FEMMESIL® Cream and FEMMESIL® Ultra Therapy Ointment are formulated with sensitive intimate skin in mind. For jock itch specifically, TERRASIL® Jock Itch Treatment MAX may be relevant regardless of gender.
What Is Balanitis — and How Is It Different from Jock Itch?

Balanitis is inflammation of the glans — the head of the penis. It’s a condition that only men can develop, and it’s more common than most people talk about. Estimates suggest that up to 10% of men will experience balanitis at some point in their lifetime, with uncircumcised men being at significantly higher risk.15
It comes up in this guide because it’s genuinely easy to confuse with jock itch, a groin yeast infection, or even herpes — especially for someone who hasn’t experienced it before. The redness, irritation, and discomfort are real, and the location is close enough to jock itch territory that the confusion is understandable. But balanitis is its own condition, with its own causes, and it responds to care differently.
What causes balanitis
Candida yeast is the most common cause — accounting for roughly 25 to 50% of cases. This is why balanitis is sometimes called candidal balanitis, or informally referred to as a penile yeast infection. The warm, moist environment under the foreskin in uncircumcised men creates ideal conditions for Candida to overgrow. But balanitis can also be caused by bacterial infections, skin irritation from harsh soaps or detergents, certain skin conditions like psoriasis or eczema, and occasionally by sexually transmitted infections.15,16
Diabetes is a significant risk factor. High blood sugar means sugar-rich urine can accumulate under the foreskin, creating a hospitable environment for yeast and bacteria. Recurring balanitis in an adult man is sometimes one of the first signals that blood sugar may not be well controlled.16
What balanitis looks like
Balanitis presents specifically on the head of the penis and, in uncircumcised men, the foreskin. The skin appears red, swollen, and may look shiny or glazed. There may be white or yellowish patches, a thick or foul-smelling discharge under the foreskin, and pain or burning during urination. The foreskin may feel tight or difficult to retract. In some cases, small papules or erosions appear on the glans.15
This is what distinguishes it clearly from jock itch: jock itch is a rash that spreads across the inner thigh and groin crease in a ring-shaped pattern — it doesn’t typically involve the head of the penis. Balanitis, on the other hand, is localized to the glans and foreskin. The location alone tells you something important.
Can balanitis spread between partners?
When balanitis is caused by Candida yeast, it can transfer back and forth between sexual partners — particularly if a female partner has a vaginal yeast infection. This is one of the reasons recurring balanitis is worth discussing with a healthcare provider, since both partners may need care simultaneously to break the cycle.16
The practical difference: Jock itch is a spreading rash on the inner thigh and groin. Balanitis is localized redness, swelling, and irritation on the head of the penis itself. If the discomfort is concentrated there rather than in the crease of the groin, balanitis is the more likely explanation — and it warrants a different approach to care.
TERRASIL® Balanitis Relief Ointment is formulated to support comfort and skin recovery for balanitis-related irritation and inflammation of the genital skin. The Serious Balanitis Relief System pairs the ointment with the Balanitis Cleansing Bar for a complete cleansing and care routine — keeping the area clean is a core part of managing and preventing balanitis recurrence.
Jock Itch and Athlete’s Foot: More Connected Than You’d Think

If you have jock itch and athlete’s foot at the same time, that’s not a coincidence — it’s actually quite common. Both are caused by the same dermatophyte fungi, and the two infections regularly appear together or fuel each other’s recurrence.
The connection works like this: the fungus living on infected feet can transfer to the groin through clothing. If you pull underwear over bare, infected feet before putting on socks, you’ve just given the fungus a ride to a warm, dark, moist new location. That’s one of the most common ways jock itch develops or keeps coming back despite treatment. The fix is simple — put socks on before underwear — but it’s something most people have never thought about.1
If you’re dealing with recurrent jock itch and also have athlete’s foot, addressing both at the same time is important. Treating the groin while leaving the feet untreated is a bit like mopping the floor with the tap still running. Using an athlete’s foot antifungal treatment alongside groin care helps break the cycle
TERRASIL® Athlete’s Foot Antifungal Ointment is formulated for tinea pedis to support clearing the fungal infection at the source. Treating athlete’s foot alongside jock itch may help break the cycle of reinfection between the two sites.
Jock Itch vs. Chafing: Friction or Fungus?
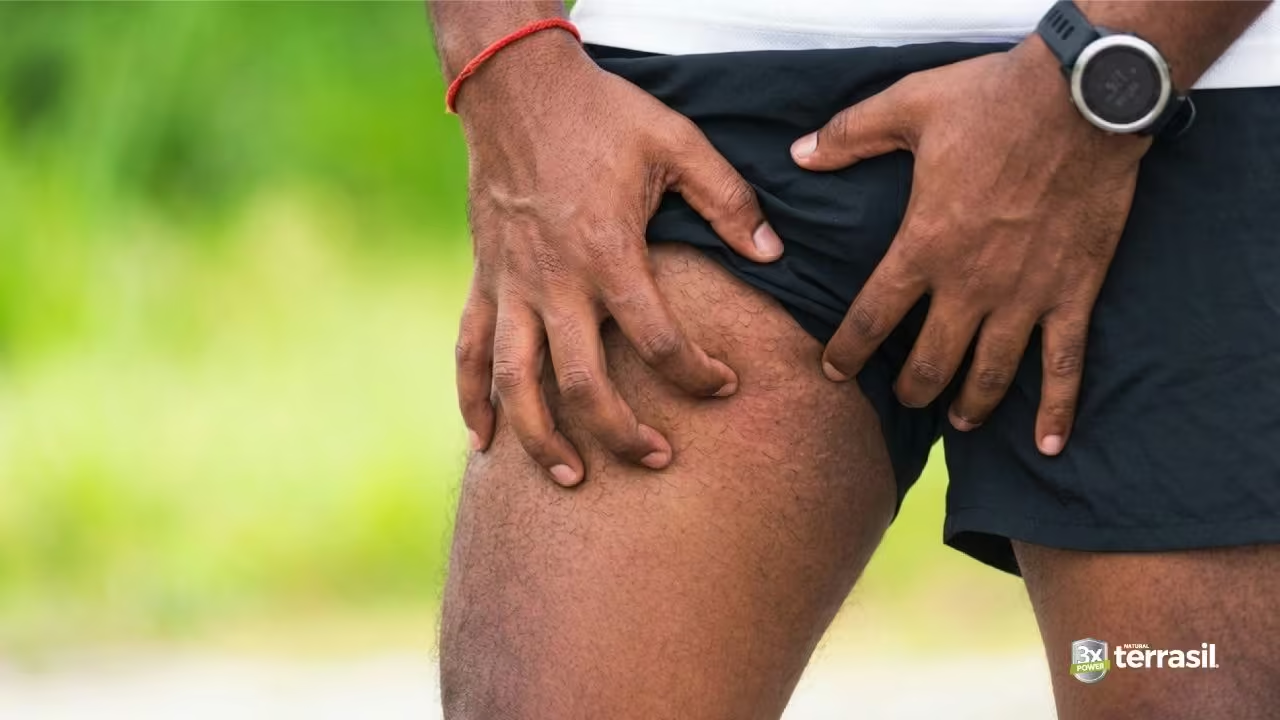
Chafing is probably the most frequently mistaken condition when it comes to jock itch. Both cause redness and irritation in the inner thigh and groin area, and both tend to flare with physical activity and sweating. If you’ve been assuming the two are basically the same thing, you’re not alone — but the causes are completely different, and so is the right approach to care.
Chafing is not an infection. Nothing is growing, nothing is spreading. It’s a purely mechanical reaction — skin rubbing against skin or fabric, wearing away the protective outer surface and leaving the area raw, red, and stinging. The discomfort is a direct response to friction. It doesn’t require antifungal treatment because there’s no fungus involved.11
The clearest way to tell them apart
Look at the border — or rather, the absence of one. Jock itch has a clearly defined, raised, scaly edge that advances as the fungus spreads. Chafing has no such border. The redness fades gradually and evenly, following the exact path where skin has been rubbing. There’s no ring, no advancing edge, no defined shape — just uniform irritation that matches the friction pattern.12
Timing also tells you something. Chafing tends to appear and resolve in direct relation to activity. A long run, a hot day in tight jeans, an intense workout — the skin gets irritated, and with rest and reduced friction, it starts to settle within a day or two. Jock itch doesn’t work that way. Rest doesn’t make it better. It lingers, and if the fungus isn’t addressed, it tends to slowly spread.
Worth knowing: Chafing that damages the skin’s surface can actually make the area more vulnerable to a fungal infection. If you’ve had persistent chafing and notice the rash starting to develop a more defined edge or ring-like shape, it’s worth considering whether a secondary fungal infection has developed on top of the original irritation.11
Understanding how friction and everyday irritants affect your skin barrier helps explain why antifungal products don’t work here.
For skin that’s been rubbed raw or irritated by friction, TERRASIL® Anti-Bacterial Skin Repair Ointment is formulated to support recovery of damaged skin and help protect the disrupted skin barrier while the area heals.
Jock Itch vs. Herpes: Addressing the Anxiety Directly

Let’s be honest about something: for a lot of people, noticing something unusual in the groin area immediately triggers anxiety about sexually transmitted infections — herpes in particular. That reaction is completely understandable. But it’s also worth knowing that jock itch and genital herpes look and behave quite differently, and once you understand the key differences, the two are easier to distinguish than the initial panic might suggest.
Jock itch is a fungal infection. Herpes is a viral infection caused by the herpes simplex virus (HSV-1 or HSV-2). They are fundamentally different in cause, appearance, sensation, and behavior — and they require entirely different approaches to care.13
What each one looks and feels like
Jock itch presents as a broad, spreading rash — ring-shaped, scaly, with that characteristic raised border spreading across the inner thigh and groin crease. The dominant sensation is itching. It may burn somewhat, especially after sweating, but pain is not its defining feature.
Herpes presents very differently. Instead of a rash, it produces clusters of small, fluid-filled blisters in a localized area. Those blisters are painful — sometimes significantly so. They eventually break open, leaving raw ulcers that crust over as they heal. The pain and tenderness are often the most prominent symptoms, and many people notice a tingling or burning sensation in the area before the blisters even appear.13
Herpes recurs. Jock itch doesn’t work that way.
Another meaningful difference: after an initial herpes infection, the virus remains in the body and can reactivate periodically — often triggered by stress, illness, or changes in immune function. Those reactivations are called outbreaks, and they follow a recognizable pattern. Jock itch doesn’t do this. It may come back if the conditions that caused it return, but it doesn’t lie dormant and re-emerge in the way a viral infection does.14
Herpes may also be accompanied during an initial outbreak by flu-like symptoms — fatigue, swollen lymph nodes, general malaise. Jock itch causes no systemic symptoms at all. It stays on the skin and doesn’t affect how you feel beyond the local discomfort.14
Either way, a healthcare provider can usually distinguish between jock itch and herpes quickly by examination, and can confirm herpes with a swab test if blisters are present. That’s always the most reliable path. Getting a clear answer is far better than guessing.
What Commonly Helps Each Condition

This is where matching the cause to the care really matters. Here’s a straightforward overview of the approaches most commonly associated with each condition. This is educational information — not medical advice — and a healthcare provider is the right resource for anything that isn’t improving or remains unclear.
For jock itch and ringworm
Because both are dermatophyte fungal infections, antifungal care is the relevant approach. Topical antifungal ingredients like clotrimazole work by disrupting the fungal cell membrane and are widely available over the counter. Consistent use over the full recommended duration matters — stopping early because the rash looks better is one of the most common reasons jock itch keeps coming back.2
Equally important is reducing the moisture environment. Keeping the area clean and thoroughly dry, wearing breathable underwear, showering promptly after physical activity, and changing out of damp clothing all support recovery and help prevent the fungus from returning.3
TERRASIL® Jock Itch Treatment MAX and the Serious Jock Itch Cure 2-Product System are formulated for tinea cruris with a paired treatment and cleansing approach. For ringworm on the body, TERRASIL® Ringworm Treatment MAX Ointment and Antifungal Treatment MAX may also be relevant depending on location and severity.
For groin yeast infections

Candidal infections may respond to antifungal care, but the type of antifungal matters — some agents are better suited to Candida specifically. Keeping the area cool, dry, and well-ventilated is particularly important, since moisture is a primary driver of yeast overgrowth. Addressing any underlying contributing factors — like completing a course of antibiotics or managing blood sugar levels — also supports recovery.9
FEMMESIL® Cream and FEMMESIL® Ultra Therapy Ointment are formulated for the sensitive external intimate skin area. The FEMMESIL® Ultra Therapy Vaginal Ointment & Cleansing Bar Kit provides a paired cleansing and topical care routine for external intimate skin concerns.
For balanitis
When balanitis is caused by Candida yeast — which is the most common cause — antifungal care applied to the affected area is the typical approach. Keeping the area clean and dry is equally important: gently cleaning under the foreskin daily and ensuring the area is thoroughly dry afterward removes the moist environment that yeast and bacteria rely on. Avoiding harsh soaps or detergents in the area helps prevent irritation-driven balanitis. Men with diabetes may find that improved blood sugar control reduces recurrence.16
TERRASIL® Balanitis Relief Ointment is formulated to support comfort and skin recovery for balanitis-related genital skin irritation. Used as part of the Serious Balanitis Relief System alongside the Balanitis Cleansing Bar, it supports both the cleansing and the care steps that are central to managing this condition.
For chafing

Chafing needs friction reduction and skin barrier support — not antifungal treatment. Keeping the area clean and dry, applying a gentle protective ointment, choosing breathable fabrics, and addressing the source of friction are the core approaches. The skin just needs a chance to recover without continued rubbing. Antifungal products have no effect on chafing because there’s no fungus to address.11
TERRASIL® Anti-Bacterial Skin Repair Ointment may help support recovery of skin that has been damaged by friction, helping protect the disrupted skin barrier while the area heals.
For herpes

Genital herpes is managed with antiviral medications, which require a prescription. Over-the-counter antifungal products have no effect on a viral infection. A healthcare provider is the right first step for anyone who suspects herpes — both for accurate identification and for access to appropriate care options.14
Prevention: What Actually Helps — By Condition Type

Prevention isn’t one-size-fits-all here. Fungal infections, yeast overgrowth, and viral infections are different organisms with different vulnerabilities — and the habits that help with one don’t always apply to another. Here’s how to think about prevention by cause, by gender, and by what to do when you’re already dealing with something active.
Preventing fungal infections (jock itch, ringworm, athlete’s foot)
Dermatophyte fungi need warmth, moisture, and an opportunity to spread. Take away any one of those and the risk drops meaningfully.
- Keep the groin area dry — shower promptly after exercise and dry the area thoroughly, including skin folds, before dressing
- Wear breathable fabrics — loose-fitting cotton or moisture-wicking underwear reduces trapped sweat and heat
- Put socks on before underwear — this prevents athlete’s foot fungus from transferring to the groin through clothing1
- Don’t share towels or clothing — dermatophyte fungi spread easily through shared textiles, even after a single use
- Change out of sweaty clothes promptly — wet fabric against skin is one of the most consistent risk factors for tinea infections
- Treat athlete’s foot if you have it — an untreated foot infection is a persistent source of reinfection for the groin
- Wear sandals in communal spaces — locker rooms, pool decks, and gym showers are common pickup sites for fungal spores
Preventing yeast infections and balanitis
Candida is already on most people’s skin. Prevention is about keeping the conditions that allow it to overgrow in check.
- Be mindful after antibiotics — antibiotics disrupt the natural balance of bacteria and yeast; this window after a course is when yeast is most likely to overgrow
- Manage blood sugar — elevated blood sugar creates conditions favorable to Candida; recurring yeast infections or balanitis can sometimes be an early signal that blood sugar is worth discussing with a provider16
- Clean under the foreskin daily — for uncircumcised men, gently cleaning and thoroughly drying under the foreskin is the single most effective prevention habit for balanitis15
- Use gentle, fragrance-free cleansers — harsh soaps and scented intimate washes are a common irritant trigger for both balanitis and intimate skin inflammation
- Avoid sugary or flavored lubricants during sex — the sugar in them can feed yeast and increase infection risk17
Gender-specific considerations
For men: Athletic supporters, cups, and compression shorts trap heat and moisture in the groin more than any other clothing type. Wash them after every single use — not every few uses. Switching from briefs to boxers reduces friction and improves airflow for men prone to recurring jock itch. During an active infection, using a dedicated towel for the groin area and a separate one for the rest of the body prevents spreading the fungus to other areas like the hands, feet, or torso.3
For women: Tight synthetic fabrics — leggings, thongs, and swimwear worn for extended periods — create a warm, moist environment in the groin that fungal and yeast infections thrive in. Cotton underwear, or breathable athletic fabric that wicks moisture away, significantly reduces that risk. Avoid lingering in wet swimwear after swimming. Scented intimate washes, douches, and even scented toilet paper can disrupt the vaginal and vulvar skin’s natural pH and microbial balance, making yeast overgrowth more likely. Plain warm water and a mild, unscented cleanser for the external area only is typically the gentler, more protective approach.
Sheets, towels, and laundry: what to do normally — and what to do when infected

This part matters more than most people realize. Fungal spores can survive on fabric for weeks, and Candida albicans has been shown to remain active on textiles for up to a month — meaning unwashed towels and sheets can reinfect you or transmit to a partner even after the original rash starts to clear.19
Normal baseline — when you’re not infected:
- Wash bath towels every 3–5 uses; allow them to fully dry between uses — a damp towel hanging on a hook is an active breeding ground for fungi and bacteria19
- Wash bed sheets weekly; wash pillowcases every 2–3 days if you have active skin concerns
- Wash underwear after every single use; wash workout clothing and athletic supporters after every use regardless
- Wash all laundry in hot water when possible — heat kills fungal spores more effectively than cold or warm cycles20
- Ensure clothing is fully dry before wearing — damp fabric provides exactly the environment fungus needs to grow
When you have an active infection — fungal or yeast:
- Wash towels after every single use — do not reuse them even once during an active infection
- Use a separate towel for the infected area and a different towel for the rest of your body; using the same towel spreads fungus from the groin to your hands, feet, or torso3
- Wash bed sheets every 2–3 days in hot water for the duration of the infection
- Change underwear at least once daily — more if you sweat; do not wear the same pair twice without washing
- Do not share any towels, clothing, or bedding with others while infected
- Wash your hands thoroughly after touching the infected area — scratching and then touching other body parts is a documented route of self-spread1
- Do not scratch — beyond the discomfort it causes, scratching transfers fungal spores under your fingernails and onto whatever you touch next
Contagiousness: what spreads, how far, and to whom
Not everything on this list spreads the same way — or at all. Understanding the actual contagiousness of each condition helps you take the right precautions without unnecessary anxiety.
Jock itch and ringworm are genuinely contagious. The fungus spreads through direct skin-to-skin contact, shared clothing, shared towels, contaminated gym equipment, and locker room surfaces. It can also spread from one part of your own body to another — from feet to groin via clothing, or from the groin to the hands via scratching. During an active infection, avoiding skin contact with others in the affected area and laundering everything aggressively are the most practical protective measures.1,3
Yeast infections are not contagious in the same way as tinea fungi, but Candida can transfer between sexual partners. A man with candidal balanitis can pass yeast to a female partner during sex, and vice versa. This is why both partners addressing an active yeast infection at the same time is sometimes necessary to break a cycle of recurrence.16
Chafing is not contagious. It is a mechanical skin reaction, not an infection. There is nothing to transmit.
Herpes is highly contagious through sexual and close skin-to-skin contact. It can transmit even when no sores are visible — the virus sheds intermittently from the skin in the absence of symptoms. During an active outbreak, avoiding sexual contact is strongly advised. Between outbreaks, consistent condom use reduces (but does not eliminate) transmission risk. Touching a sore and then touching another part of your body or another person’s skin without washing hands can also spread the virus. Daily suppressive antiviral therapy, taken consistently, has been shown to significantly reduce both outbreak frequency and the risk of transmitting herpes to a partner.13,14
Diet and its role in yeast overgrowth
There is a well-established link between high blood sugar and Candida overgrowth — which is why diabetes is consistently identified as one of the most significant risk factors for yeast infections and balanitis. What’s less settled in the research is whether dietary sugar directly affects skin Candida in people without diabetes.
What the evidence does support: diets consistently high in refined sugars and heavily processed foods may raise blood glucose and disrupt the balance of beneficial bacteria in the gut and on the skin — both of which can create conditions more favorable to Candida overgrowth. Alcohol metabolizes similarly to sugar in the body and may play a comparable role. A diet higher in fiber, whole foods, and lean protein supports the microbial balance that keeps Candida in check.18
The practical takeaway: if you deal with recurring yeast-related infections and your diet is consistently high in sugar, refined carbohydrates, or alcohol, that pattern is worth paying attention to. It won’t replace antifungal care — but it may support it and reduce how often infections come back.
Worth knowing: Diet alone is rarely sufficient to clear an established yeast infection. But if infections keep recurring despite care, blood sugar and lifestyle factors are worth discussing with a healthcare provider. Recurring infections can sometimes be an early indicator of pre-diabetes or other conditions worth checking.
Safe sex: before, during, and after
Different conditions spread differently, and the sexual transmission picture isn’t the same for all of them.
Jock itch and ringworm are not sexually transmitted infections in the clinical sense, but the fungus can transfer through close skin-to-skin contact. Avoiding sexual contact during an active, untreated infection is a reasonable precaution.3
Yeast infections and balanitis caused by Candida can transfer between partners through unprotected sex. Using barrier methods during an active yeast infection, waiting until symptoms have fully cleared before resuming sex, and both partners addressing the infection simultaneously all reduce back-and-forth reinfection.17
Herpes requires a more careful ongoing approach. The virus can shed and transmit even without visible sores — which means the risk isn’t limited to visible outbreaks. Before sex, open communication with a partner about HSV status is the foundation of informed consent. During sex, consistent use of condoms or dental dams significantly reduces transmission risk, though herpes can spread through skin-to-skin contact in areas not fully covered. After sex, gentle cleansing and washing hands thoroughly are sensible habits. For people with known herpes, daily suppressive antiviral therapy has been shown to reduce both outbreaks and the risk of transmitting to partners by over 90% in some studies.13,14
- Before sex: know your status, communicate openly, and avoid sexual activity during any active outbreak or unresolved infection
- During sex: use barrier methods consistently; choose pH-friendly, unscented lubrication; avoid flavored products near the genitals
- After sex: gently cleanse the genital area with a mild, unscented cleanser; dry thoroughly; wash hands
Frequently Asked Questions
Conclusion
Dealing with an itchy, red rash in the groin or inner thigh area is uncomfortable enough without the added stress of not knowing what you’re looking at. The good news is that once you know the key differences — the border, the texture, the location, the pattern of symptoms, what makes it worse — the picture becomes much clearer.
Jock itch and ringworm are fungal infections that respond to antifungal care. A groin yeast infection is caused by a different organism and looks different from tinea. Balanitis affects the head of the penis specifically and has its own causes and care approach. Chafing is pure friction with no infection involved, and it improves with rest and friction reduction. Herpes is a viral infection that causes painful blisters — a very different presentation from any of the fungal conditions. These aren’t subtle distinctions once you know what to look for.
If something still isn’t adding up after reading this — or if a rash isn’t responding to care as expected — a healthcare provider can confirm the cause quickly and point you in the right direction. You don’t have to keep guessing.
This article is intended for informational and educational purposes only and does not constitute medical advice. Always read and follow product label directions. If you are uncertain about a skin condition or the appropriate care approach for your situation, consult a qualified healthcare professional.
References
1 Cleveland Clinic – Jock Itch (Tinea Cruris)
https://my.clevelandclinic.org/health/diseases/22141-jock-itch-tinea-cruris
2 Merck Manual Professional – Tinea Cruris (Jock Itch) — October 2025
https://www.merckmanuals.com/professional/dermatologic-disorders/fungal-skin-infections/tinea-cruris-jock-itch
3 WebMD – Jock Itch: Causes, Treatment, Prevention — May 2024
https://www.webmd.com/men/causes-and-prevent-jock-itch
4 Harvard Health Publishing – Jock Itch (Tinea Cruris) — October 2023
https://www.health.harvard.edu/a_to_z/jock-itch-tinea-cruris-a-to-z
5 Patient.info – Fungal Groin Infection (Tinea Cruris) — January 2025
https://patient.info/infections/fungal-infections/fungal-groin-infection-tinea-cruris
6 CDC – Ringworm
https://www.cdc.gov/fungal/diseases/ringworm/index.html
7 StatPearls / NCBI – Tinea Cruris
https://www.ncbi.nlm.nih.gov/books/NBK554602/
8 DermNet NZ – Candidal Intertrigo — January 2025
https://dermnetnz.org/topics/candidiasis-of-skin-folds
9 Merck Manual Consumer – Candidiasis (Yeast Infection) — October 2025
https://www.merckmanuals.com/home/skin-disorders/fungal-skin-infections/candidiasis-yeast-infection
10 Cleveland Clinic – Intertrigo — August 2023
https://my.clevelandclinic.org/health/diseases/21693-intertrigo
11 Cleveland Clinic – Chafing — August 2023
https://my.clevelandclinic.org/health/diseases/23517-chafing
12 GoodRx – Jock Itch: Treatments and Symptoms — April 2025
https://www.goodrx.com/conditions/fungal-infection/jock-itch-tinea-cruris-prevention
13 CDC – Genital Herpes
https://www.cdc.gov/std/herpes/default.htm
14 Mayo Clinic – Genital Herpes
https://www.mayoclinic.org/diseases-conditions/genital-herpes/symptoms-causes/syc-20356161
15 StatPearls / NCBI – Balanitis — August 2024
https://www.ncbi.nlm.nih.gov/books/NBK537143/
16 Cleveland Clinic – Balanitis
https://my.clevelandclinic.org/health/diseases/21186-balanitis
17 Evvy – Yeast Infection After Sex — January 2026
https://www.evvy.com/blog/yeast-infection-after-sex
18 PMC / NCBI – Healthy Diet and Lifestyle Improve the Gut Microbiota and Help Combat Fungal Infection
https://pmc.ncbi.nlm.nih.gov/articles/PMC10302699/
19 Cleveland Clinic – How Often Should You Wash Your Bath Towels?
https://health.clevelandclinic.org/how-often-should-you-wash-your-germ-magnet-of-a-bath-towel
20 Kaiser Permanente – Jock Itch Care Instructions
https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.jock-itch-care-instructions.uh4967




 Jock Itch System ↗
Jock Itch System ↗ Tinea System ↗
Tinea System ↗ femmesil® System ↗
femmesil® System ↗ Balanitis System ↗
Balanitis System ↗ Skin Repair ↗
Skin Repair ↗ Terragen™ HG Formula ↗
Terragen™ HG Formula ↗



