Last Updated: March 2026
This article is reviewed periodically to reflect current dermatology information and treatment approaches.
If you’ve been searching for what ringworm looks like, there’s a good chance you’re looking at a rash right now and trying to figure out what it might be.
Maybe it’s a small, itchy patch. Maybe the edges look slightly raised, or a faint circle seems to be forming. When something unusual appears on your skin, it’s natural to feel uncertain — especially when it doesn’t look like something you’ve seen before.
Ringworm is one of the most common fungal skin infections worldwide, but it often surprises people because it rarely looks the way they expect.
Despite the name, ringworm has nothing to do with worms. The infection is caused by fungi called dermatophytes, which live on the outer layer of the skin.¹
Ringworm is extremely common and very treatable, even though it may look concerning at first.
What makes ringworm confusing is that its appearance changes as it develops. A rash that looks like dry skin or mild irritation today may look very different in a week.
Understanding how ringworm develops — and how the rash changes during different stages — can help explain what you may be seeing on your skin. Because ringworm can resemble other skin conditions in its early stages, identifying its visual patterns can help you distinguish it from eczema, irritation, or other common rashes.
Quick Answer: What Does Ringworm Look Like?
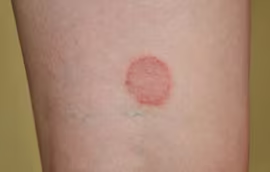
Ringworm typically appears as a circular rash with a red or raised border and clearer center. The rash may itch, flake, or slowly expand outward as the fungal infection spreads across the outer layer of the skin.
Our Commitment to Accurate, Evidence-Based Information
Our articles are written using information from peer-reviewed dermatology research and reputable health organizations. We review scientific literature and clinical resources to ensure the information we share is clear, accurate, and helpful.
Sources referenced in this article include materials from organizations such as the Centers for Disease Control and Prevention (CDC) and the American Academy of Dermatology.
Key Takeaways
- Ringworm is a fungal skin infection that often forms a circular rash with a raised border.
- The infection is caused by dermatophyte fungi, primarily from the genera Trichophyton, Microsporum, and Epidermophyton.
- The infection usually begins as a small irritated patch before gradually spreading outward.
- Ringworm can appear on many areas of the body, including arms, legs, scalp, groin, and feet.
- Antifungal ingredients such as clotrimazole are commonly used to address fungal skin infections.
- The rash may change appearance as the infection spreads and as the skin begins recovering.
What Ringworm Looks Like in the Early Stages

In the beginning, ringworm often looks subtle and easy to dismiss.
Many people first notice something like:
- a small reddish patch
- slightly dry or irritated skin
- mild itching that comes and goes
- a faint flaky texture
At this stage, the rash may only be about the size of a coin.
Because early symptoms can resemble common skin irritation, many people assume it is simply dry skin or a temporary rash that will disappear on its own.
However, fungal infections behave differently from ordinary irritation.
Dermatophyte fungi feed on keratin, a protein found in the outer layer of skin, hair, and nails.¹ As long as keratin is available and the environment remains warm and moist, the fungi can continue spreading outward.
This is why a small patch that looks harmless at first may gradually expand over time.
Why Ringworm Forms a Ring
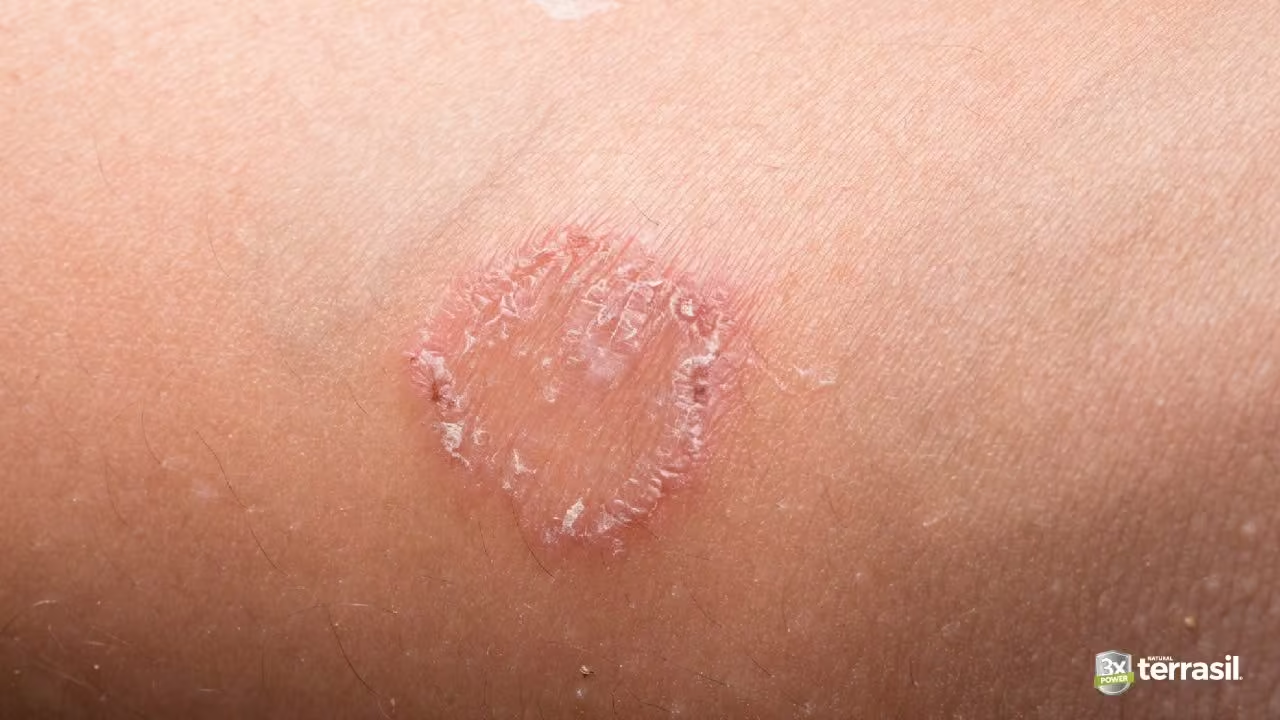
The circular shape of ringworm isn’t random — it reflects how the infection spreads.
Dermatophyte fungi grow outward from the original point of infection.
As the fungi expand across the skin:
- The outer edge remains active, where the fungi are still growing
- The center may begin calming, as the body responds to the infection
This contrast creates the familiar pattern:
- a red or raised outer ring
- calmer skin toward the center
That pattern is what gives ringworm its name.²
Not every infection forms a perfect circle. Some appear oval or slightly irregular, depending on how the fungi spread across the skin.
The Classic Ringworm Rash
As the infection progresses, the rash often becomes easier to recognize.
Typical features may include:
- a circular or oval shape
- a raised or red border
- dry or flaky skin
- itching or irritation
The outer edge of the rash often appears more inflamed because that is where the fungal growth is most active.
Meanwhile, the center of the rash may look calmer or closer to normal skin tone.
Ringworm Stages: How the Rash Changes as It Spreads and Heals
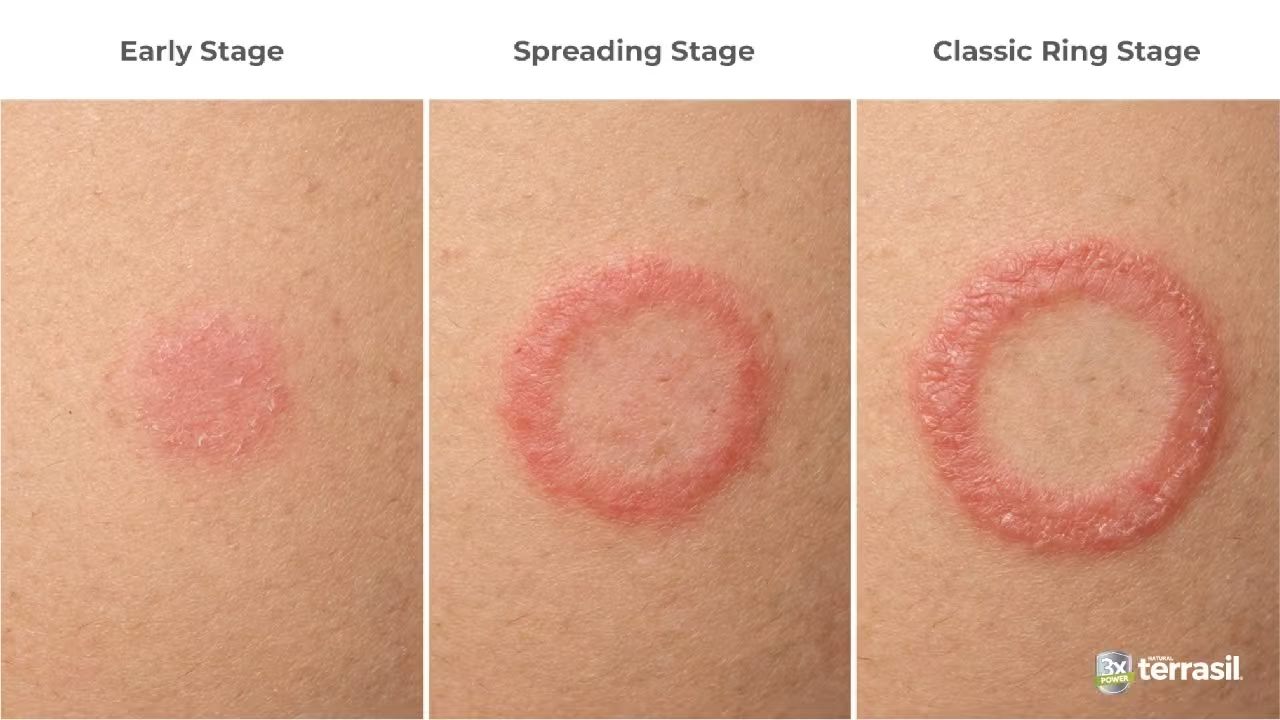
Ringworm doesn’t stay the same throughout the infection. The rash often changes gradually as the fungi spread and the skin begins responding.
Early stage
The infection may begin as a small irritated patch that resembles dry skin or a mild rash.
Spreading stage
The rash gradually expands outward as fungal growth continues across the skin. The border becomes more defined while the center may begin calming.
Classic ring stage
The circular rash becomes more recognizable, often with a red border and clearer center.
Healing stage
As antifungal treatment addresses the infection, the rash may slowly fade. The border may stop expanding, and redness may gradually improve as the skin recovers.
Because the infection affects the outermost layer of the skin, visible improvement can occur gradually as the skin replaces affected cells.
Common Places Ringworm Appears
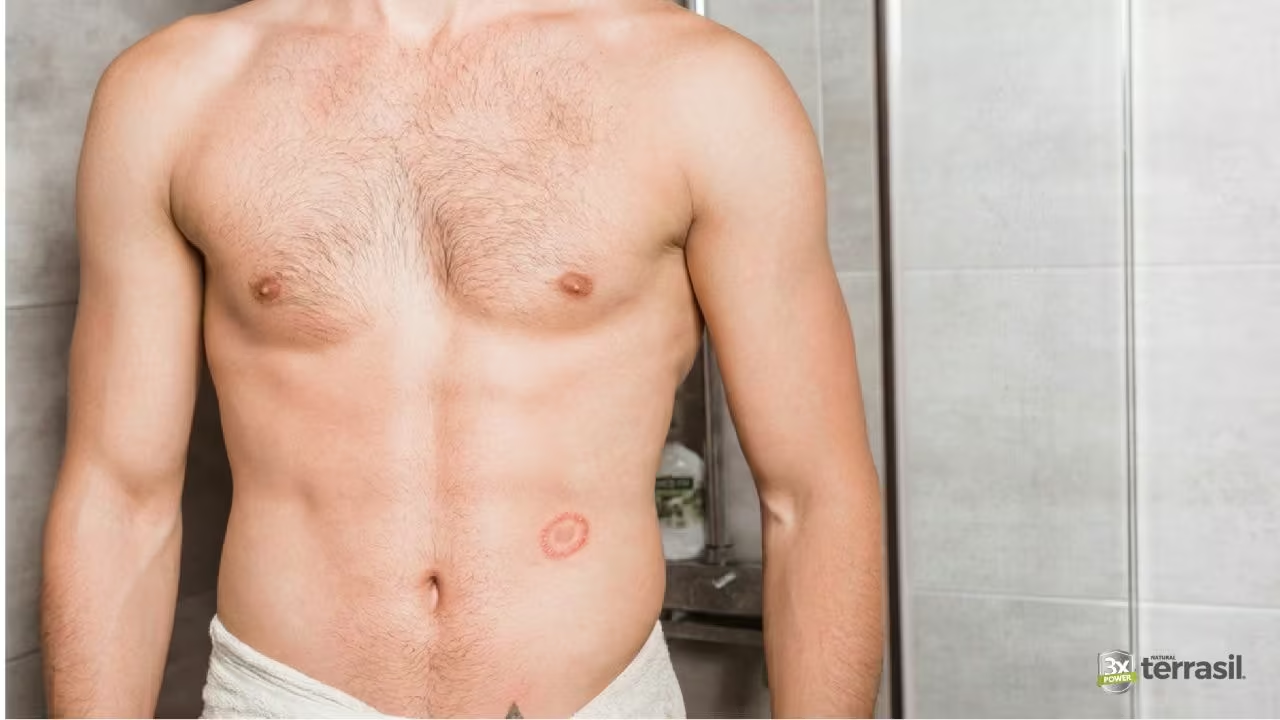
Ringworm can appear on many areas of the body.
Common locations include:
- arms
- legs
- torso
- neck
- face
- scalp
- groin
- feet
Some infections have different names depending on where they appear. For example, athlete’s foot affects the feet, while jock itch affects the groin. Although the names differ, these infections are caused by the same types of dermatophyte fungi.³
Where People Commonly Catch Ringworm

Ringworm spreads through fungal spores that can survive on surfaces and fabrics.
People may encounter these spores in environments such as:
- gyms and locker rooms
- communal showers
- shared sports equipment
- shared towels or clothing
- wrestling mats or athletic facilities
Because fungi thrive in warm and humid environments, shared spaces where skin contact occurs can sometimes allow the infection to spread more easily.³
What Causes Ringworm
Ringworm is caused by dermatophyte fungi that grow on the outer layer of the skin.
These fungi feed on keratin, a structural protein found in skin, hair, and nails.¹
The infection can spread through:
- direct skin-to-skin contact
- contaminated surfaces
- shared clothing or towels
- infected animals such as cats or dogs
Fungal skin infections, including ringworm, athlete’s foot, and jock itch, affect millions of people worldwide each year.⁴
Which Fungi Cause Ringworm? The Dermatophytes Explained
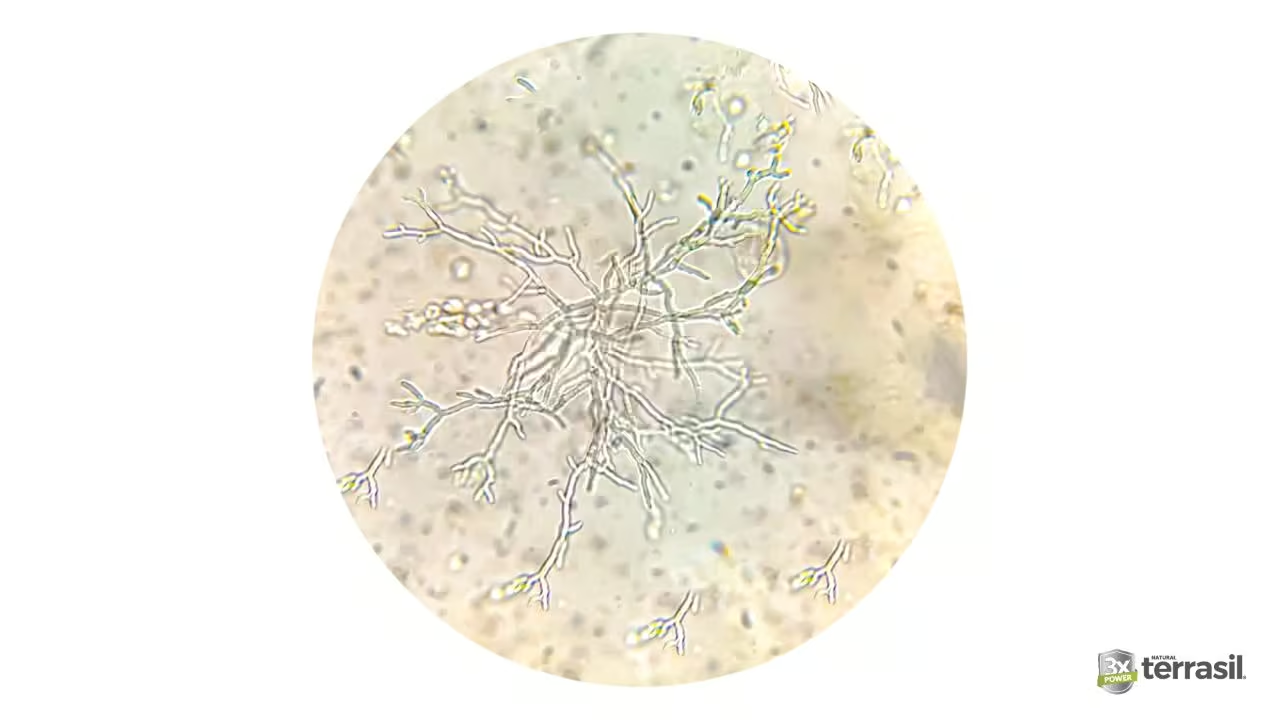
“Ringworm” is not caused by a single organism. It is a general term for a fungal skin infection that can be triggered by roughly 40 species of dermatophytes, though a small number of species account for the vast majority of cases worldwide.⁵
Dermatophytes are organized into three main genera, each with distinct characteristics:
Genus | Key characteristic | Common species |
|---|---|---|
Trichophyton | The most frequent cause of ringworm in humans globally | T. rubrum, T. tonsurans |
Microsporum | Often transmitted from animals such as cats and dogs | M. canis |
Epidermophyton | Primarily affects the skin and nails; less commonly the scalp | E. floccosum |
The Most Common Species
While many species can cause ringworm, three tend to be responsible for the majority of infections:
- Trichophyton rubrum — the leading cause of ringworm worldwide, particularly for infections on the body, feet, and nails.⁵
- Trichophyton tonsurans — a major cause of scalp ringworm, especially in children in the United States.⁵
- Microsporum canis — frequently seen in children who have close contact with infected pets such as cats or dogs.⁵
How Ringworm Is Named by Body Location
Medical professionals use the term tinea followed by a Latin descriptor to specify where on the body the infection is located. This naming system helps standardize diagnosis and treatment, even though the same dermatophyte species may be responsible across different sites.
Tinea corporis
Ringworm on the body (arms, legs, or trunk)
Tinea capitis
Ringworm on the scalp; can cause itchy, flaky patches or hair loss
Tinea pedis
Commonly known as athlete’s foot
Tinea cruris
Commonly known as jock itch
Tinea unguium
Fungal infection of the nails (also called onychomycosis)
Tinea faciei
Ringworm on the face
How Ringworm Is Diagnosed
In many cases a doctor can identify ringworm from its appearance alone. When additional confirmation is needed, two methods are commonly used:
- Potassium Hydroxide (KOH) test — a skin scraping is examined under a microscope after applying a KOH solution, which dissolves skin cells and makes fungal elements easier to identify.⁶
- Fungal culture — a sample is grown in a laboratory over several days or weeks to confirm the specific species causing the infection.⁶
For scalp ringworm, a Wood’s lamp (ultraviolet light) may also be used, as some Microsporum species fluoresce under UV light.⁶
What Actually Kills Ringworm
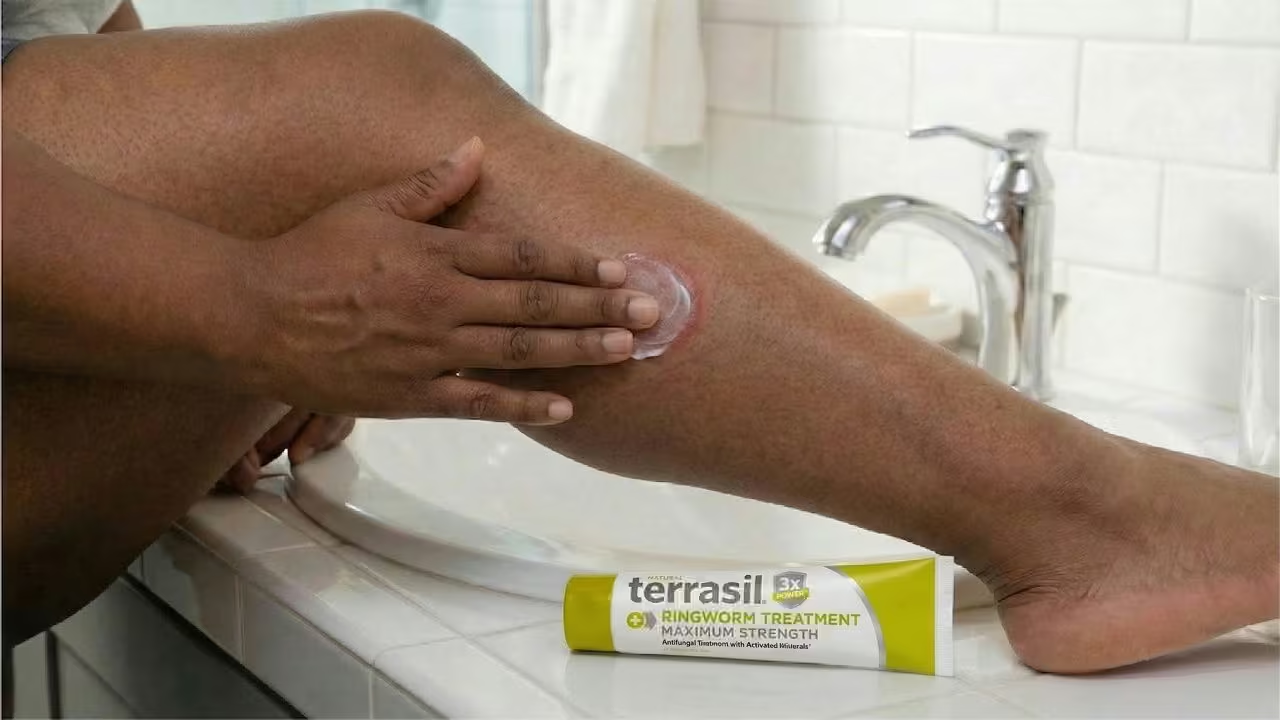
Ringworm is commonly addressed with antifungal ingredients designed to stop fungal growth.
Common antifungal APIs include:
- clotrimazole
- terbinafine
- miconazole
- tolnaftate
These ingredients interfere with fungal growth by disrupting the fungal cell membrane or blocking essential enzymes the fungi need to survive.²·⁷ Because dermatophytes live in the outer layers of the skin, consistent topical application is typically required over a period of several weeks to fully address the infection. Starting treatment promptly and following through the full recommended course can make a meaningful difference in how the infection resolves.
If you’re comparing treatment options, our guide Best Ringworm Cream – What Actually Works explains how the most common antifungal ingredients differ.
Why the Formula of a Ringworm Cream Matters

Many antifungal treatments contain the same active ingredient — clotrimazole. However, the overall formulation can vary significantly between products.
Some antifungal creams focus primarily on delivering the active ingredient alone. Others are designed to support the condition of the skin throughout the treatment process.
Terrasil® Ringworm Treatment MAX Ointment with Activated Minerals® contains clotrimazole as the antifungal API, but the formulation also includes Activated Minerals® technology and targeted botanical ingredients.
Activated Minerals® are included to help create a protective environment on the skin’s surface, supporting skin comfort while the antifungal ingredient is applied.
The formula also contains botanical ingredients selected for their skin-conditioning properties.
Because antifungal treatments are typically applied consistently for several weeks, many people prefer formulas designed to help maintain skin comfort and hydration during the treatment process.
A well-formulated product isn’t only about the active ingredient — it also considers how the skin feels during the treatment period.
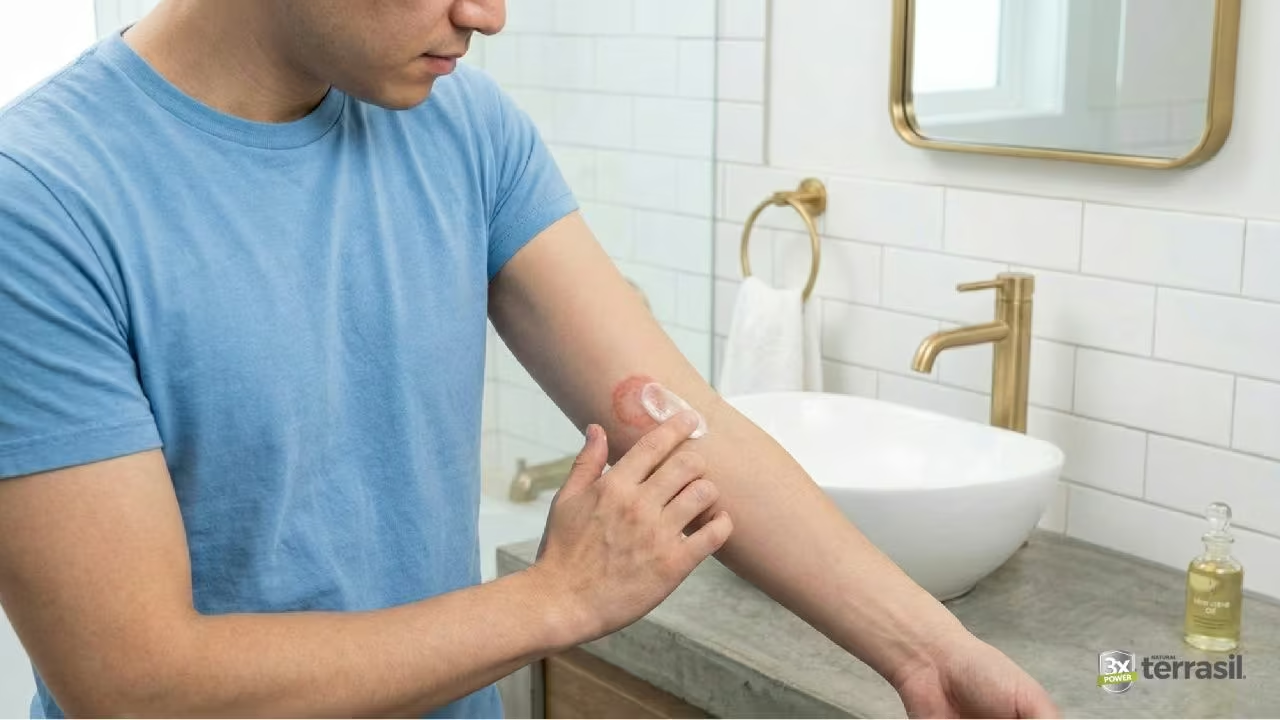
Preparing the Skin Before Applying Treatment

Before applying antifungal treatment, cleansing the affected area can help remove sweat, oils, and debris from the skin.
Some people use cleansing bars designed for fungal skin concerns.
Terrasil® Ringworm Cleansing Bar contains moisturizing ingredients like olive oil and shea butter along with botanical ingredients including tea tree oil and peppermint oil. It also contains Activated Minerals® designed to support skin comfort during cleansing.
After washing and thoroughly drying the skin, antifungal treatment can be applied according to product directions.
Many antifungal treatments are typically applied twice daily, often once in the morning and once in the evening.
How Ringworm Changes as It Heals
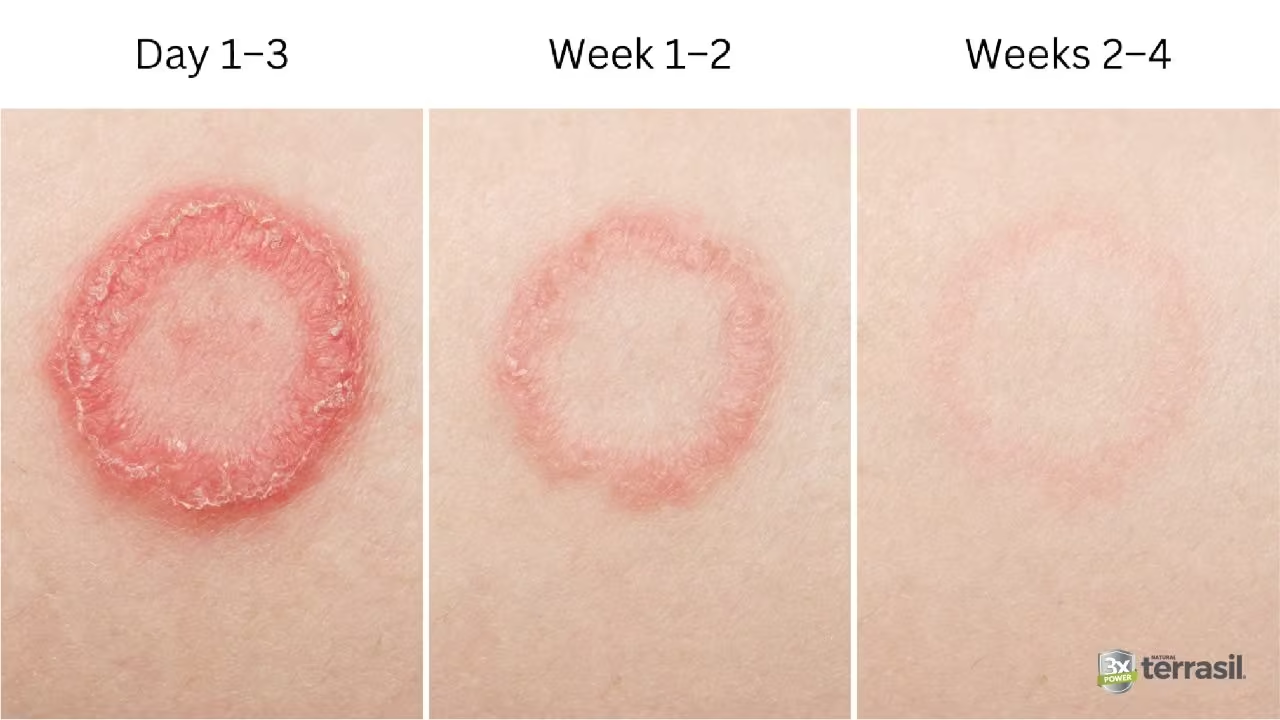
As treatment addresses the infection, the rash may gradually improve.
Common signs of improvement include:
- less itching
- fading redness
- shrinking borders of the rash
- reduced scaling or flaking
The outer border may stop expanding as the skin begins recovering.
Because the infection affects the outer layer of the skin, visible improvement may take time as new skin cells replace the affected ones.
Simple Habits That Help Prevent Ringworm

Some everyday habits can help reduce exposure to fungal spores.
Helpful practices include:
- keeping skin clean and dry
- changing sweaty clothing promptly
- washing workout gear regularly
- avoiding shared towels or clothing
- wearing footwear in communal showers
These habits help reduce the warm, moist environments where fungi tend to grow.
Frequently Asked Questions
Conclusion
If you’re wondering what ringworm looks like, the infection often begins as a small irritated patch that gradually spreads outward.
Over time the rash may develop the circular pattern that ringworm is known for — a shape that directly reflects how dermatophyte fungi expand across the skin.
Understanding which fungi are responsible and how the infection changes during its different stages can help explain why the rash may evolve as the skin responds and recovers.
References
- Centers for Disease Control and Prevention (CDC). Ringworm and Fungal Nail Infections. https://www.cdc.gov/ringworm/
- American Academy of Dermatology Association. Ringworm: Signs, Symptoms, and Treatment. https://www.aad.org/public/diseases/a-z/ringworm-overview
- Mayo Clinic. Ringworm (Tinea Corporis): Symptoms and Causes. https://www.mayoclinic.org/diseases-conditions/ringworm-body/symptoms-causes/syc-20353780
- Hay R., et al. Tinea Corporis (Ringworm of the Body). StatPearls Publishing, National Center for Biotechnology Information (NCBI). https://www.ncbi.nlm.nih.gov/books/NBK544360/
- Zhan P., et al. Dermatophytosis: A Review of Species Distribution and Epidemiology. Mycopathologia. https://doi.org/10.1007/s11046-021-00544-2 [For genus/species prevalence data: T. rubrum, T. tonsurans, M. canis.]
- Ely J.W., Rosenfeld S., Seabury Stone M. Diagnosis and Management of Tinea Infections. American Family Physician. 2014;90(10):702–710. https://www.aafp.org/pubs/afp/issues/2014/1115/p702.html [KOH test, fungal culture, Wood’s lamp.]
- Gupta A.K., Versteeg S.G. Topical Treatment of Superficial Dermatophyte Infections. Clinical Dermatology Reviews. https://journals.lww.com/cddr
This article is intended for informational purposes only and is not medical advice. Always read and follow product label directions. Consult a healthcare professional if you are uncertain about a skin condition or treatment.































 Pro Tip: If a pet is scratching, grooming excessively, or shows patchy hair loss, ringworm may be involved — humans and pets can pass the fungus back and forth.
Pro Tip: If a pet is scratching, grooming excessively, or shows patchy hair loss, ringworm may be involved — humans and pets can pass the fungus back and forth.


 If symptoms worsen or fail to improve after 4 weeks, escalation is needed.
If symptoms worsen or fail to improve after 4 weeks, escalation is needed.