Last Updated: April 2026
Reviewed periodically to reflect current dermatology and women’s health information
Anyone who’s had a vaginal yeast infection knows exactly what it feels like — and “uncomfortable” doesn’t begin to cover it. The burning is constant. The itch is relentless. You can’t sit still, you can’t focus, and if you’ve ever stood in a cold shower just to get a few seconds of relief, you’re not being dramatic — that’s exactly how bad it can get. In severe cases it’s genuinely debilitating: walking hurts, clothing hurts, sleeping hurts.
And although yeast infections are not only found in women and their vagina, it counts among the most common intimate skin conditions — up to 75% of women will have at least one infection in their lifetime, and nearly half will have two or more.1 And yet they’re frequently misidentified, mistreated, and confused with bacterial vaginosis, contact dermatitis, and other conditions that look and feel similar but aren’t the same.
This guide covers everything: what a yeast infection looks and feels like, where on the body it can appear, what causes it, how men can get it too, whether it can spread to other parts of your body, natural approaches that may help, and which ones are myths. Because when you’re that uncomfortable, you deserve real information — not vague reassurance.
At a Glance
Yeast infection symptoms on the skin usually include intense itching, redness, swelling, burning, and irritation in warm or moist areas of the body. While most people associate yeast infections with the vagina, Candida can also affect skin folds, the groin, under the breasts, and even men.
A yeast infection is caused by an overgrowth of Candida yeast — most commonly Candida albicans — on the skin and mucous membranes. The external skin symptoms most commonly include:
- Intense, relentless itching of the vulva, labia, and surrounding skin
- Redness and swelling of the vulva and labia
- A burning sensation, especially during urination or sex
- Thick, white, odorless discharge that may resemble cottage cheese
- Soreness and rawness of the external intimate skin
- Small fissures or cracks in the skin in more severe cases
These symptoms can range from mild and manageable to genuinely disruptive. They also appear in other conditions — which is why identifying the full picture matters.1,2
Key Takeaways
- Yeast infections affect external intimate skin — the vulva, labia, and surrounding area — not just the inside of the vagina
- Candida can cause infections anywhere on the body: mouth, skin folds, under the breasts, nails — not just the intimate area
- Men can get yeast infections too — including from sexual contact with an infected partner
- Discharge from a yeast infection is typically thick, white, and odorless — unlike BV, which has a distinctive fishy smell
- Natural approaches like probiotics and diet changes may support prevention, but they don’t replace antifungal care for an active infection
- Gentle external intimate cleansing supports skin comfort during and after a yeast infection — harsh products make symptoms worse
- Recurring yeast infections may signal an underlying factor worth discussing with a healthcare provider
Our commitment to accurate, evidence-based information: This article draws on peer-reviewed research and trusted health organizations, including the CDC, WHO, Cleveland Clinic, Mayo Clinic, MedlinePlus, NCBI/StatPearls, and the Office on Women’s Health. All sources are numbered and linked in the references section below.
Where Can a Yeast Infection Appear on the Body?
Candida is not just a vaginal problem. It’s a yeast that lives naturally on the skin and inside the body — in the mouth, digestive tract, skin folds, and vagina — and it can overgrow in any warm, moist environment on or inside your body. Most people associate yeast infections exclusively with the vagina, but the same organism is responsible for infections in all of these locations.11
Mouth (Thrush)
White raised patches on tongue or inside cheeks. Often follows antibiotic use.
For most healthy people, a yeast infection stays localized — it affects one area rather than spreading throughout the body. Systemic or invasive candidiasis, where Candida enters the bloodstream and spreads to internal organs, is a serious medical condition that occurs almost exclusively in people who are critically ill, hospitalized, or have severely weakened immune systems — not in otherwise healthy individuals.12
External vs. Internal Symptoms: Why the Distinction Matters
When most people think of a yeast infection, they think of internal symptoms — discharge and internal discomfort. But a significant part of a yeast infection’s impact is external, happening right on the surface of the intimate skin. This distinction matters for two reasons.
First, the external symptoms are often what you notice first and feel most acutely. The itching, redness, and swelling of the vulva and labia are visible and felt directly on the surface. Second, external care — gentle cleansing, soothing the skin — is a meaningful part of comfort management that often goes unaddressed when people focus only on internal treatments.
A yeast infection affects both. The vaginal lining is involved internally, and the vulva, labia majora, labia minora, and surrounding skin are involved externally. Candida thrives in warm, moist skin folds, which is why the external intimate area is particularly vulnerable.4
External Skin Symptoms: What You Can Actually See and Feel
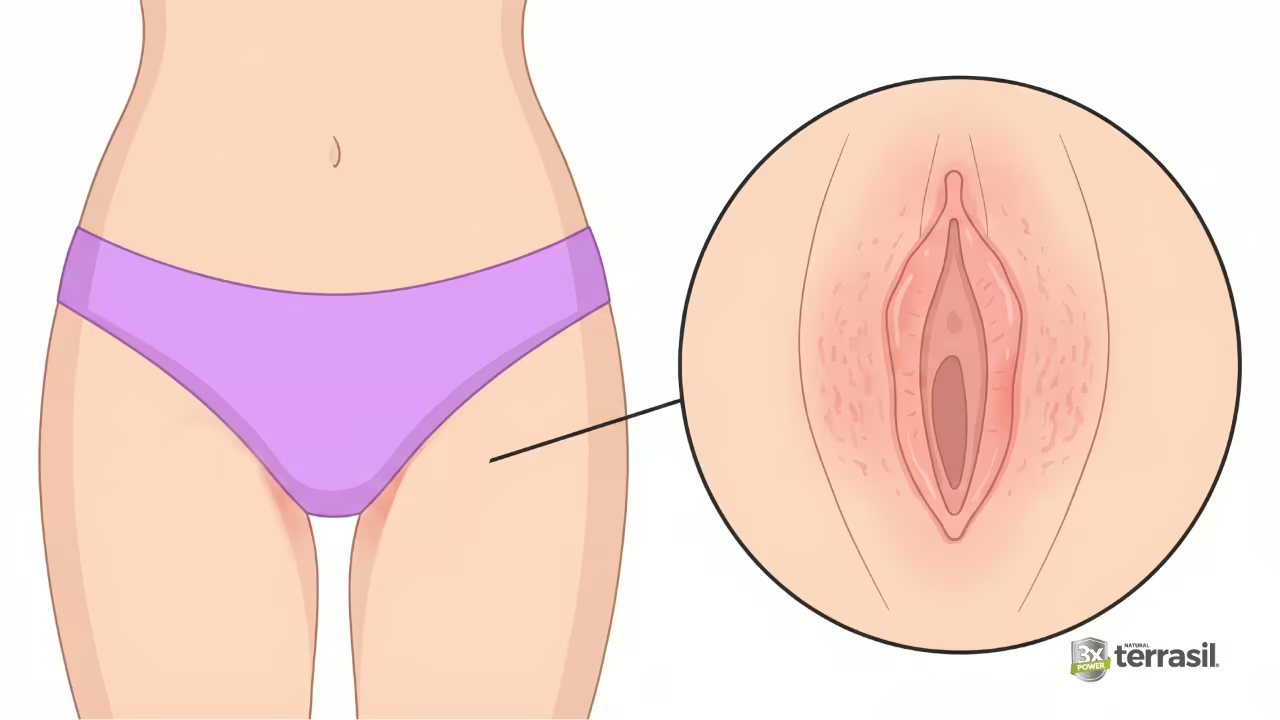
These are the symptoms that show up on the outside — on the vulva, labia, and surrounding skin. They’re the ones that cause the most day-to-day discomfort and the ones that a good external care routine can most directly address.
Intense itching
The itching associated with a yeast infection isn’t subtle. It tends to be persistent, often worsening at night, and can range from a nagging irritation to a genuinely disruptive sensation that makes it hard to focus on anything else. The itching is caused by the inflammatory response to Candida overgrowth — your immune system reacting to the fungus on the skin’s surface.1
Scratching may momentarily relieve the sensation, but it worsens the underlying inflammation, damages the skin barrier further, and can introduce bacteria into already irritated tissue. It also spreads the yeast to surrounding skin. Resisting the urge to scratch — easier said than done — is one of the most protective things you can do for the skin while it heals.
Redness and swelling of the vulva and labia
The external intimate skin becomes visibly inflamed. The vulva — which includes the labia majora (outer folds), labia minora (inner lips), and clitoral hood — may appear red, swollen, and irritated. In some cases the labia look noticeably puffy. This redness and swelling is the skin’s inflammatory response to the Candida overgrowth, and it can extend slightly beyond the vulva into the surrounding groin folds.1,4
The CDC’s clinical guidelines specifically note that severe cases may present with extensive vulvar redness, swelling, and excoriation — meaning the skin may appear scratched or broken from irritation alone, even without direct scratching.2
Burning sensation
Burning is one of the most reported external symptoms. It tends to intensify in two specific situations: during urination, when urine contacts the already-inflamed vulvar skin, and during or after sexual intercourse, when friction aggravates the irritated tissue. Neither of these is a sign that the infection is spreading — they’re a reflection of how inflamed and sensitive the external skin has become.1
If urination is particularly painful, it’s worth ruling out a urinary tract infection (UTI) with a healthcare provider, as UTIs can occur alongside yeast infections and have overlapping symptoms.
Discharge
The discharge associated with a yeast infection is a reliable distinguishing feature. It’s typically thick, white, and odorless — often described as resembling cottage cheese in texture, though it can also be watery in milder cases. The absence of odor is significant: a strong or fishy smell points away from a yeast infection and toward bacterial vaginosis.3,5
The discharge itself doesn’t cause damage, but its presence on the external skin can increase moisture, which further irritates already-inflamed tissue. Gentle cleansing of the external area to remove discharge without disrupting the skin barrier is a practical comfort measure.
Soreness, rawness, and skin fissures
In more significant cases, the external skin may feel genuinely raw — sore to the touch, sensitive to clothing, and uncomfortable with movement. Small fissures or cracks can develop in the skin of the vulva and labia, particularly where the skin folds meet. These fissures are painful and increase vulnerability to secondary infection if left unaddressed.2
The CDC classifies yeast infections with extensive vulvar redness, swelling, excoriation, and fissure formation as “severe VVC” — these cases typically need a longer course of care and benefit most from prompt evaluation by a healthcare provider.
Yeast Infections in Skin Folds: Under the Breasts and Beyond

That persistent red rash under the breasts, in abdominal folds, or between the inner thighs is often dismissed as heat rash or sweat irritation. But in many cases, it’s a Candida yeast infection — the same organism, the same overgrowth mechanism, just a different address on the body.
The medical term is cutaneous candidiasis or candidal intertrigo when it occurs in skin folds. Typical areas affected include the inframammary fold (under the breasts), abdominal folds, the groin, the armpits, and between the fingers and toes.13 The reason skin folds are so vulnerable is straightforward: warmth, moisture, and limited airflow create exactly the environment Candida needs.
What it looks like
The rash is bright red — more intensely red than a typical heat rash — and the skin looks wet or shiny rather than dry. It sits deep in the fold and may extend slightly beyond it. One of the most characteristic features is the presence of satellite pustules: small red bumps scattered just beyond the main rash border. The area may itch, burn, or feel sore, and in more significant cases, the skin may look white and softened from prolonged moisture exposure — a state called maceration. 4
How to tell it apart from heat rash
Heat rash produces tiny, uniform pink or clear bumps and typically clears on its own once the skin cools and dries. A candidal skin fold rash doesn’t clear with cooling alone. It persists, may slowly worsen, and has that characteristic intensely red, wet appearance with satellite pustules at the edges. If a skin fold rash has been present for more than a few days without improvement, Candida is worth considering.
Who is more susceptible
People with larger or pendulous breasts, higher BMI, diabetes, those who sweat heavily, and those in hot or humid climates are all at elevated risk. This isn’t about hygiene — it’s about anatomy and the conditions the skin creates in certain fold areas, regardless of care habits.4
For external intimate skin folds, FEMMESIL® Cream and FEMMESIL® Ultra Therapy Ointment are formulated to support soothing comfort for sensitive external skin. For non-intimate skin fold locations — under the breasts or in abdominal folds — TERRASIL® Antifungal Treatment MAX may be relevant as an antifungal support option.
Can Men Get a Yeast Infection?

Yes — absolutely. Candida doesn’t care about gender. Men can and do develop yeast infections, typically presenting as candidal balanitis: inflammation of the head of the penis and, in uncircumcised men, the foreskin. It’s less commonly discussed than vaginal yeast infections, but it’s far from rare. Estimates suggest that 3–11% of men will develop a yeast infection at some point in their lifetime.14
If you or someone you know is dealing with balanitis, TERRASIL® Balanitis Relief Ointment is formulated specifically for the redness, irritation, and discomfort associated with genital skin inflammation. For a more complete care approach, the Serious Balanitis Relief System pairs the ointment with the TERRASIL® Balanitis CleansingBar — because keeping the area gently cleansed is just as important as topical care when it comes to managing balanitis and reducing the likelihood of it coming back. The cleansing bar is formulated to clean the sensitive skin of the glans and foreskin without the harsh ingredients that commonly aggravate already-inflamed tissue.
To learn more about balanitis, read our full guide: What Causes Balanitis? A Complete Breakdown of Triggers and Risk Factors.
Can a man get a yeast infection from an infected woman during sex?
Yes, though it’s not common, and yeast infections are not classified as sexually transmitted infections. When a male partner has unprotected sex with a woman who has an active yeast infection, Candida can be transferred. Studies suggest that around 15% of male partners of women with a yeast infection may develop penile symptoms following exposure.8 This is one reason that avoiding sexual activity during an active infection and waiting until symptoms have fully cleared is recommended for both partners.
What do men experience?
Male yeast infection symptoms typically appear on the head (glans) of the penis and the foreskin. The signs include:
- Redness and swelling of the glans
- Itching and burning under the foreskin
- A shiny, glazed, or white appearance to the skin of the glans
- White discharge under the foreskin
- Tightness or difficulty retracting the foreskin in uncircumcised men
- Pain or burning during urination or sex in more significant cases8
How else can men get a yeast infection?
Sexual contact isn’t the only route. Men develop yeast infections through the same mechanisms as anyone else:
- Antibiotic use — depletes the bacteria that keep Candida in check across the body
- Diabetes or high blood sugar — elevated glucose in body fluids creates favorable conditions for Candida to overgrow, particularly under the foreskin where sugar-rich urine can accumulate8
- Being uncircumcised — the warm, moist environment under the foreskin is inherently more hospitable to yeast
- A weakened immune system — from illness, HIV, corticosteroid medications, or other immunosuppressive conditions
- Poor hygiene under the foreskin — not cleaning thoroughly allows debris and moisture to accumulate
- Wearing tight, non-breathable clothing — traps heat and moisture in the groin
Recurring balanitis in men: If a man keeps developing yeast infections and doesn’t have an obvious trigger like recent antibiotics, it’s worth checking blood sugar. Recurring candidal balanitis is sometimes among the first signs of undiagnosed pre-diabetes or poorly managed diabetes.8
Can a Yeast Infection Travel to Other Parts of Your Body?
This is a question a lot of people have and don’t always get a clear answer to. The short answer: in healthy people, a vaginal or skin yeast infection very rarely “travels” internally to other organs. But Candida can and does appear at multiple sites on the body — sometimes at the same time — and the direction of spread matters.
Surface-to-surface spread
Candida can spread from one warm, moist area of the skin to another through direct contact. Scratching an infected area and then touching another part of the body can transfer the yeast. A vaginal yeast infection can potentially spread to the surrounding perianal skin, inner thighs, and groin folds if the area remains moist and hygiene practices allow cross-contamination. Oral thrush can spread to the throat and esophagus in people with weakened immune systems. Handwashing after touching any infected area is a practical protective measure.13
Can it come from the gut?
Candida naturally lives in the gut as well as on the skin. There is some evidence suggesting that gut Candida overgrowth may contribute to the likelihood of vaginal yeast infections by increasing the overall load of Candida in the body — particularly in people who have recently taken antibiotics that disrupted gut flora. This is part of why probiotic research focuses on both oral and vaginal administration routes.15
Systemic spread — serious but rare in healthy people
In people with severely compromised immune systems — those undergoing chemotherapy, with advanced HIV, in intensive care, or on immunosuppressive medications — Candida can enter the bloodstream and spread to internal organs including the kidneys, heart, eyes, and brain. This is called invasive or systemic candidiasis, and it is a medical emergency requiring urgent treatment. For otherwise healthy people, this scenario is extremely unlikely.12
The practical takeaway: don’t panic about “spreading,” but do practice good hygiene, address active infections promptly, and if you notice Candida symptoms in multiple body areas simultaneously — for example, thrush plus a vaginal infection plus a skin fold rash — it’s worth discussing with a healthcare provider, as that pattern sometimes indicates an underlying immune or blood sugar issue worth investigating.12
What Causes Yeast to Overgrow?
Candida is already there. The question is always what tips the balance. These are the most common factors that allow it to overgrow.
Antibiotic use
The most common trigger. Antibiotics kill bacteria — including the beneficial Lactobacillus bacteria that normally keep Candida in check in the vagina. When those protective bacteria are depleted, Candida has the opportunity to multiply rapidly. If a yeast infection starts within days of finishing antibiotics, that’s why.3
Hormonal changes
Estrogen influences the vaginal environment, and fluctuations affect the balance of bacteria and yeast. Pregnancy significantly raises estrogen — which is why pregnant people are at considerably higher risk. Oral contraceptives, hormone therapy, and the days before a menstrual period when estrogen drops are all common triggers.5,6
Diabetes and blood sugar
Elevated blood sugar creates an environment that favors Candida growth. People with uncontrolled or poorly managed diabetes are significantly more susceptible, and recurring infections can sometimes be an early indicator that blood sugar levels need attention.4
A weakened immune system
A healthy immune system keeps Candida populations regulated. When immunity is compromised — through illness, certain medications like corticosteroids, or conditions such as HIV — the body’s ability to keep yeast in balance decreases.3
Warmth, moisture, and tight clothing
Wearing tight synthetic underwear, staying in wet swimwear or sweaty workout clothes, and high-humidity environments all create exactly the environment yeast prefers.6
Intimate products and douching
Scented soaps, vaginal deodorants, douches, and scented intimate washes disrupt the natural pH and microbial balance of the vagina and vulvar skin. The vagina is self-cleaning and doesn’t need any of these products. Using them removes the beneficial bacteria that protect against yeast overgrowth, making infections more likely rather than less.6
How External Yeast Infection Symptoms Differ from Other Conditions

Several conditions produce symptoms similar enough to a yeast infection that they’re regularly mistaken for one — and treated incorrectly as a result.
Feature | Yeast Infection | Bacterial Vaginosis (BV) | Contact Dermatitis | Trichomoniasis |
|---|---|---|---|---|
Main symptom | Intense itching, burning, redness | Discharge with fishy odor — itching less prominent | Itching, redness, rawness at point of contact | Itching, burning, frothy discharge |
Discharge | Thick, white, odorless — cottage cheese texture | Thin, gray or white, strong fishy odor | None typically | Frothy, yellow-green, foul-smelling |
Odor | None or very mild yeasty smell | Pronounced fishy odor, especially after sex | None | Strong, unpleasant odor |
External skin | Red, swollen vulva and labia — may have fissures | Minimal external changes | Redness exactly where irritant contacted | Redness, swelling, irritation |
Cause | Candida yeast overgrowth | Bacterial imbalance in vaginal microbiome | Allergic or irritant reaction to a product | Parasite — sexually transmitted |
Contagious? | Not typically — can transfer between partners | Not an STI but linked to sexual activity | No | Yes — sexually transmitted |
Yeast infection vs. bacterial vaginosis
BV is the most common vaginal condition in people ages 15 to 44 — and also the most frequently confused with a yeast infection.5 The key distinguishing feature is discharge and odor. A yeast infection produces thick, white, odorless discharge. BV produces thin, gray or white discharge with a pronounced fishy smell. Itching dominates with yeast; odor dominates with BV. The treatments are completely different — BV requires antibiotics, not antifungal care.5
Yeast infection vs. contact dermatitis
Scented soaps, laundry detergents, wet wipes, latex condoms, lubricants, and intimate hygiene products can all trigger contact dermatitis of the vulvar skin — a reaction that looks and feels very similar to a yeast infection. The difference: contact dermatitis has no discharge, no odor, and the irritation appears right where the product contacted the skin. Remove the offending product and improvement follows. A yeast infection won’t improve without antifungal care.7
Yeast infection vs. trichomoniasis
Trichomoniasis causes genital itching and burning similar to a yeast infection, but the distinction is in the discharge — frothy, yellow-green, and foul-smelling. Trichomoniasis requires specific antibiotic treatment, and both partners need to address it simultaneously.3
First time having these symptoms? Seeing a healthcare provider is the most reliable next step. Studies show that up to two-thirds of women who self-diagnose a yeast infection actually have a different condition — so getting a confirmed identification before self-treating is always the safer call.1
Symptoms in Women vs. Men
The yeast infection conversation is heavily female-skewed — but Candida can cause external intimate skin symptoms in men too, typically as candidal balanitis (inflammation of the head of the penis). Men who are uncircumcised, have diabetes, or have recently taken antibiotics are at higher risk.
In men, the external symptoms include redness and swelling of the glans, itching and burning under the foreskin, a shiny or glazed appearance to the skin, and sometimes a white discharge under the foreskin. The sensation is similar — the warm, moist environment under the foreskin is as hospitable to Candida as vulvar skin folds.8
If you’ve read our related article on jock itch vs. yeast infection, you’ll recognize this as candidal balanitis — we cover it in depth there, including how it differs from jock itch in the inner thigh and groin.
Recurring Yeast Infections: When It Keeps Coming Back

Having four or more yeast infections in a year is classified as recurrent vulvovaginal candidiasis (RVVC), and it affects approximately 10–20% of people who get yeast infections.2 If this sounds familiar, it’s worth taking seriously rather than just managing each episode in isolation.
Recurring infections often point to an underlying factor that isn’t being addressed — uncontrolled blood sugar, a less common Candida species that doesn’t respond to standard care, hormonal fluctuations, ongoing antibiotic use, or a partner who may be reintroducing yeast. Sometimes the vaginal microbiome is simply more susceptible to imbalance than average.2
A healthcare provider can assess what’s driving the pattern — including taking a culture to identify the specific Candida species involved — and may recommend a longer or different course of care, or strategies to reduce recurrence over time.
Recurring infections and blood sugar: If you’re having frequent yeast infections and haven’t had your blood sugar checked recently, it’s worth mentioning to a provider. Recurring yeast infections are sometimes among the first recognizable signs of pre-diabetes or poorly managed diabetes.4
Natural Approaches That May Help

When you’re in the thick of a yeast infection, it’s natural to want to try anything. Before you reach for whatever TikTok suggested, here’s what the evidence actually says about natural approaches — what may genuinely help, what’s a waste of time, and what could make things worse.
Probiotics — the most evidence-based natural option
Probiotics, specifically Lactobacillus strains, are the most researched natural approach for yeast infections. The vaginal microbiome is normally dominated by Lactobacillus bacteria, which keep Candida in check by producing lactic acid and competing for adhesion sites. When that balance is disrupted — by antibiotics, hormones, or illness — Candida can fill the gap.
Research published in 2024 in the Journal of Clinical Medicine reviewed 25 clinical studies and seven systematic reviews and found that probiotics offer “a generally positive yet inconsistent” picture for managing yeast infections — promising as a supportive or preventive strategy, but not consistently effective as a standalone treatment.15 The strains most studied include Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14, which have shown particular promise for vaginal health.
Importantly, oral probiotics can actually reach the vagina — research has confirmed that specific Lactobacillus strains taken by mouth were recovered from vaginal samples within one week of oral intake.16 Look for probiotics specifically formulated for vaginal health rather than general gut health formulas, and discuss with a healthcare provider if you’re prone to recurring infections.
Natural approaches may support comfort or prevention, but they should not replace antifungal treatment for an active infection.
Cutting sugar and refined carbohydrates
Candida feeds on sugar — this is well established in laboratory settings and clinically meaningful for people with diabetes, where elevated blood sugar is one of the strongest risk factors for yeast infections. For people without diabetes, the direct evidence that dietary sugar causes vaginal yeast infections is less definitive, but the relationship is plausible. Diets consistently high in refined sugars and processed foods may raise blood glucose and disrupt the microbial balance that keeps Candida in check.
Reducing added sugar, refined carbohydrates, and alcohol — which metabolizes similarly to sugar — may support a healthier internal environment. This isn’t going to clear an active infection on its own, but it’s a reasonable supportive habit, especially for people with recurrent infections. Plain Greek yogurt (with live cultures, no added sugar) is a practical food choice that adds Lactobacillus to your diet without feeding yeast.17
Eating yogurt (the right kind, the right way)
Eating plain, unsweetened yogurt with live active cultures adds beneficial Lactobacillus bacteria to your gut — which may support the overall microbial balance that influences vaginal health. Some studies have found an association between regular yogurt consumption and reduced yeast infection frequency, though the evidence is mixed.17
The key: it must be plain, unsweetened yogurt with confirmed live cultures. Flavored yogurts and those with added sugar don’t offer the same benefit — and the added sugar may actually feed Candida.
Cold water relief
Running cold water over the external vulvar area — in a shower or with a gentle spray — can provide temporary, immediate relief from the burning and itching of a yeast infection. It reduces local inflammation momentarily. It doesn’t treat the infection, but there’s nothing wrong with using it for short-term comfort while you address the underlying cause. Just make sure to dry the area thoroughly afterward — residual moisture is counterproductive.
The Role of Gentle Cleansing in External Intimate Skin Care

One of the most overlooked aspects of managing yeast infection symptoms is how the external skin is cleansed — before, during, and after an infection. This matters more than most people realize.
The vulva and surrounding skin are among the most sensitive on the body. The vagina itself is self-cleaning and requires nothing other than the natural processes already happening inside it. The external vulvar skin benefits from gentle, plain cleansing — but harsh soaps, scented products, and excessive washing do more harm than good.6
During an active yeast infection, the skin is already inflamed and compromised. Using scented soaps, medicated wipes, or heavily fragranced products on irritated vulvar skin can intensify the burning and discomfort. The goal during an infection is to keep the external area clean, remove discharge gently, and avoid anything that further disrupts the skin barrier.
FEMMESIL® Vaginal Cleansing Soap Bar is formulated for gentle external intimate cleansing, free from harsh ingredients that commonly irritate sensitive vulvar skin. The FEMMESIL® Ultra Therapy Vaginal Ointment & Cleansing Bar Kit pairs this gentle cleansing step with topical comfort support as part of a complete external intimate care routine.
What May Help External Yeast Infection Symptoms

External symptoms — the itching, burning, redness, and swelling of the vulvar skin — may benefit from targeted external care while antifungal treatment addresses the underlying infection.
Antifungal care
Topical antifungal medications — containing ingredients like clotrimazole, miconazole, or terconazole — are the standard approach for addressing the underlying yeast overgrowth. They are available over the counter. Completing the full course of care, even when symptoms improve early, is important to prevent recurrence.2
External intimate skin comfort
While antifungal care addresses the infection, the external skin also benefits from specific support. Gentle cleansing, avoiding scratching, wearing breathable cotton underwear, and applying a soothing external formulation can help manage the discomfort of inflamed vulvar skin while recovery takes place.
FEMMESIL® Cream is formulated to provide comfort support for external intimate skin concerns, including the redness, irritation, and sensitivity associated with intimate skin discomfort. FEMMESIL® Ultra Therapy Ointment is a richer formulation for more significant external intimate skin irritation, designed to soothe and support the skin barrier of the vulvar area for longer periods of time. Both are formulated with sensitive, intimate skin in mind and are intended for external use only.
Keeping the area dry and cool
Moisture is what Candida thrives on. During an active infection, keeping the external intimate area as dry and cool as possible helps limit conditions favorable to further yeast growth. Change out of damp clothing promptly, dry the area gently but thoroughly after bathing, wear breathable cotton underwear, and sleep without underwear if comfortable to allow airflow.
Avoiding irritants
During a yeast infection, the external skin barrier is compromised and particularly vulnerable. Avoid scented products, douches, intimate sprays, latex condoms if sensitive to latex, fragranced lubrication, and any new skincare products in the area until the skin has fully recovered.6
Myths vs. Truths About Yeast Infections

There is a remarkable amount of misinformation circulating about yeast infections — from well-meaning advice passed down through generations to outright dangerous TikTok trends. Here’s what’s true, what’s false, and what you should never, ever do.
Myth: Putting yogurt inside your vagina treats a yeast infection.
Truth: This is one of the most persistent myths in women’s health. The Lactobacillus acidophilus in store-bought yogurt is a different species from the Lactobacillus strains that naturally populate the healthy vagina — and inserting it vaginally doesn’t produce the beneficial effect people hope for. Worse, even unsweetened yogurt contains natural sugars that can actually feed Candida. Eat yogurt with live cultures as part of a healthy diet. Don’t put it in your vagina.18
Myth: Only women who are sexually active get yeast infections.
Truth: Yeast infections are not an STI and are not caused by sexual activity. They can develop in anyone — including people who have never been sexually active. The causes are internal: antibiotic use, hormonal changes, blood sugar levels, tight clothing, moisture. Sexual activity can occasionally influence the vaginal environment, but it’s not a prerequisite for infection.3
Myth: Garlic inserted vaginally will kill the yeast.
Truth: There is no credible clinical evidence that inserting garlic vaginally treats a yeast infection. Garlic can cause significant burning and irritation on already-inflamed tissue, and introduces bacteria into the vaginal environment — the opposite of helpful. Do not put garlic in your vagina.18
Myth: If you’ve had a yeast infection before, you can always self-diagnose accurately.
Truth: Studies show that up to two-thirds of women who believe they have a yeast infection based on symptoms — including those who’ve been previously diagnosed — actually have a different condition. BV, contact dermatitis, and other infections can produce near-identical symptoms. Self-treating the wrong condition delays appropriate care. If symptoms don’t improve after standard antifungal care, or if you’re unsure, see a provider.1
Myth: Apple cider vinegar douches or baths cure yeast infections.
Truth: There is little to no clinical evidence that apple cider vinegar treats yeast infections. Applying it directly to already-inflamed intimate skin causes burning and irritation. Douching with any substance — including vinegar — disrupts the vaginal microbiome and consistently increases the risk of further infection rather than reducing it.18
Myth: Men can’t get yeast infections.
Truth: Men can and do get yeast infections, typically as candidal balanitis affecting the head of the penis and foreskin. They can develop one through sexual contact with an infected partner, through antibiotic use, high blood sugar, or being uncircumcised. It’s less common in men but far from impossible.8
Myth: A yeast infection always causes thick white discharge.
Truth: Not always. In milder cases, the discharge may be watery or absent entirely. Some yeast infections are primarily external — burning, itching, and redness without significant discharge. The absence of thick white discharge doesn’t rule out a yeast infection, just as its presence doesn’t confirm one.1,2
Prevention: Reducing the Risk of Future Infections

Many yeast infections are genuinely preventable with consistent habits. These aren’t complicated — they’re mostly about supporting the natural environment of the intimate skin rather than disrupting it.
- Wear breathable cotton underwear — synthetic fabrics trap heat and moisture; cotton allows airflow and keeps the vulvar area drier
- Change out of wet or sweaty clothing promptly — wet swimwear and sweaty workout clothes create exactly the warm, moist conditions Candida prefers
- Avoid scented intimate products — scented soaps, wipes, douches, and sprays disrupt the natural pH and bacterial balance of the vulvar area
- Never douche — the vagina self-regulates; douching removes protective bacteria and consistently increases the risk of both yeast infections and BV6
- Be mindful after antibiotics — if you’re prone to yeast infections after antibiotic courses, mention this to your provider before starting a new course
- Manage blood sugar — for people with diabetes or pre-diabetes, keeping blood sugar controlled is one of the most impactful preventive steps4
- Consider targeted probiotics — probiotic supplements containing Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14 have the most supporting research for vaginal health specifically; discuss with a healthcare provider if you experience frequent infections15,16
- Wipe front to back — prevents transfer of bacteria from the rectal area to the vaginal opening
- Choose gentle, unscented lubricants — flavored or scented lubricants can feed yeast and alter vaginal pH
- Reduce added sugar and processed foods — particularly relevant for those with recurring infections or pre-diabetes
Frequently Asked Questions
Conclusion
A yeast infection isn’t just an internal condition, and it isn’t just a woman’s problem. The external skin symptoms — the burning, itching, redness, and swelling that make it genuinely hard to function — deserve as much attention as what’s happening internally. And Candida itself can appear anywhere on the body where conditions allow, not just the vaginal area.
Understanding what those symptoms look and feel like, what causes them, how men can be affected, how the infection behaves across the body, and which natural approaches have real evidence behind them makes it significantly easier to respond appropriately — and to recognize when something you’ve read on the internet is actually going to make things worse.
Pair any antifungal care with a gentle, supportive external intimate skin routine. Eat well. Support your microbiome. And if symptoms are severe, persist after care, or keep returning, a healthcare provider is always the right next step. You don’t have to just keep managing it — you can get to the bottom of it.
This article is intended for informational and educational purposes only and does not constitute medical advice. Always read and follow product label directions. If you are uncertain about a skin condition, a diagnosis, or the appropriate care approach for your situation, consult a qualified healthcare professional. Femmesil® products are intended for external use only.
References
1 Cleveland Clinic – Vaginal Yeast Infection — May 2025
https://my.clevelandclinic.org/health/diseases/5019-vaginal-yeast-infection
2 CDC – Vulvovaginal Candidiasis (VVC) STI Treatment Guidelines
https://www.cdc.gov/std/treatment-guidelines/candidiasis.htm
3 MedlinePlus – Vaginitis (Vulvovaginitis)
https://medlineplus.gov/vaginitis.html
4 DermNet NZ – Candidal Intertrigo — January 2025
https://dermnetnz.org/topics/candidiasis-of-skin-folds
5 MedlinePlus – Vulvovaginitis
https://medlineplus.gov/ency/article/000897.htm
6 Mayo Clinic – Vaginitis: Symptoms and Causes
https://www.mayoclinic.org/diseases-conditions/vaginitis/symptoms-causes/syc-20354707
7 WebMD – Do I Have a Yeast Infection or Something Else?
https://www.webmd.com/women/do-i-have-a-yeast-infection
8 Cleveland Clinic – Male Yeast Infection (Candida Balanitis)
https://my.clevelandclinic.org/health/diseases/23199-male-yeast-infection
9 NCBI / InformedHealth.org – Vaginal Yeast Infection (Thrush) Overview — April 2022
https://www.ncbi.nlm.nih.gov/books/NBK543220/
10 Office on Women’s Health – Vaginal Yeast Infections — October 2025
https://www.womenshealth.gov/a-z-topics/vaginal-yeast-infections
11 Merck Manual – Candidiasis (Yeast Infection) Skin Disorders — October 2025
https://www.merckmanuals.com/home/skin-disorders/fungal-skin-infections/candidiasis-yeast-infection
12 Cleveland Clinic – Invasive Candidiasis — November 2025
https://my.clevelandclinic.org/health/diseases/22308-invasive-candidiasis
13 MedlinePlus – Candida Infection of the Skin
https://medlineplus.gov/ency/article/000880.htm
14 WebMD – Symptoms of a Yeast Infection — April 2024
https://www.webmd.com/women/common-symptoms-of-a-yeast-infection
15 Journal of Clinical Medicine – Probiotics in the Management of Vulvovaginal Candidosis — August 2024
https://pmc.ncbi.nlm.nih.gov/articles/PMC11396221/
16 Frontiers in Cellular and Infection Microbiology – Use of Probiotic Lactobacilli in the Treatment of Vaginal Infections
https://pmc.ncbi.nlm.nih.gov/articles/PMC10106725/
17 Healthline – Can You Treat a Yeast Infection with Yogurt?
https://www.healthline.com/health/yogurt-for-yeast-infection
18 Cleveland Clinic – Do Home Remedies Actually Work for Yeast Infections? — May 2025
https://health.clevelandclinic.org/do-home-remedies-actually-work-for-yeast-infections








