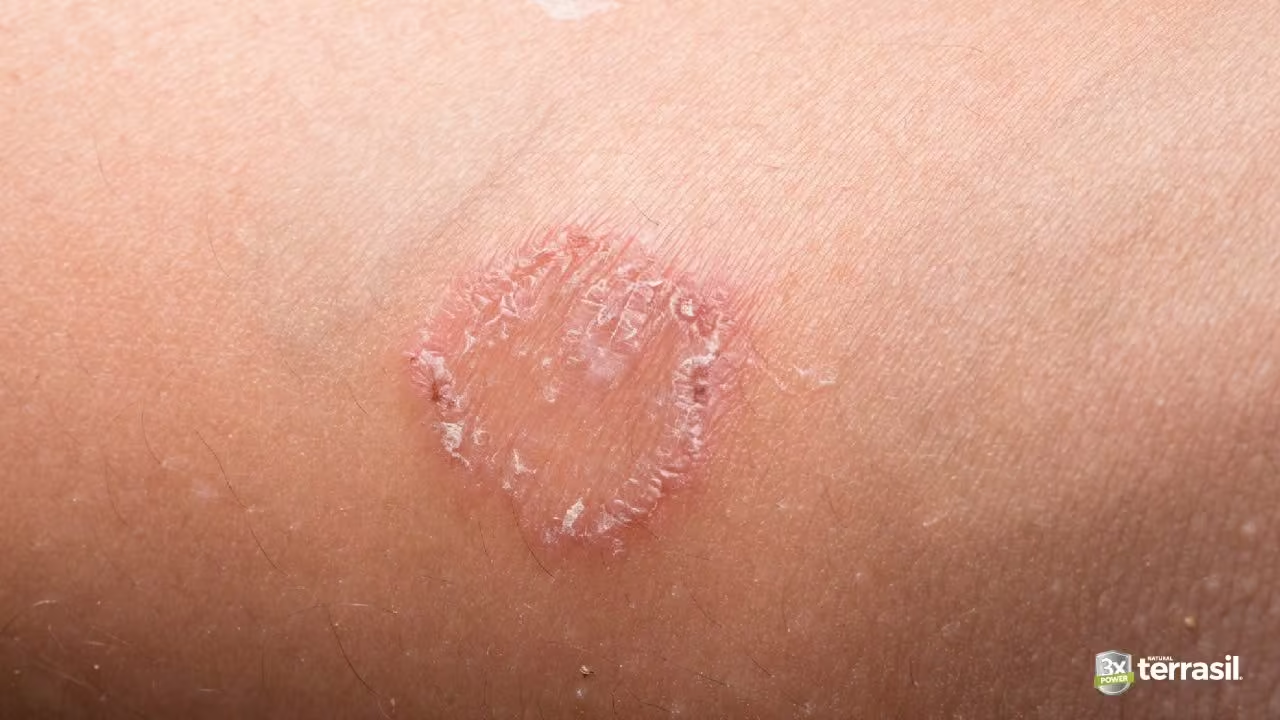
If you’ve noticed a red, circular rash spreading across your skin, you might be wondering: how long does ringworm last? If you’re searching for answers, you’re not alone. Ringworm is one of the most common fungal skin infections people encounter, and the questions that follow are always the same—”How long will this take to go away?” and “Will it ever fully clear?”
The short answer is that ringworm doesn’t disappear overnight. With consistent antifungal treatment, many people begin to see meaningful improvement within the first few weeks. Let’s explore exactly what to expect during the healing process so you can set realistic expectations and understand why patience is such an important part of recovery.
What Causes Ringworm and Why Does It Take So Long?

Before we talk about healing timelines, it helps to understand what ringworm actually is—because despite its name, it has nothing to do with worms at all.
What Actually Causes Ringworm
Ringworm is a fungal skin infection caused by organisms called dermatophytes. Despite the name “ringworm,” there are no worms involved. Instead, you’re dealing with tiny fungi—microscopic organisms that live on the outer layer of your skin. These fungi feed on keratin, a natural protein found in your skin, hair, and nails [1].
The fungi create that characteristic circular rash with a raised, scaly border and often a clearer center—which is how the infection got its misleading name. The circular, ring-like pattern made people think worms were involved, and the name stuck even though we now know it’s purely fungal.
Where Ringworm Comes From and How You Contract It
Ringworm spreads through contact with fungal spores—microscopic particles released by infected fungi. You can catch ringworm from:
Direct Contact:
- Infected people — Touching the skin of someone who has ringworm
- Infected animals — Cats, dogs, and other animals can carry ringworm spores. Petting an infected animal or handling them without washing your hands afterward is a common source of infection
- Your own infected skin — Scratching a ringworm rash and then touching another part of your body spreads the infection to new areas
Indirect Contact (Contaminated Items):
- Towels and washcloths —
Using a towel that an infected person used, or that touched their infected skin - Bedding and sheets —
Sleeping on contaminated pillows, sheets, or blankets - Clothing —
Wearing infected clothing, especially items that touch the skin like underwear or fitted shirts - Shared bathroom surfaces —
Shower floors, bathtub surfaces, and bathroom counters where spores can survive - Gym equipment and locker rooms —
Weight benches, yoga mats, shower floors, and benches where athletes change clothes - Shared personal items —
Combs, hairbrushes, razors, nail clippers, sports equipment, or helmets - Floors and communal spaces —
Swimming pools, locker rooms, and warm, moist areas where people walk barefoot - Sports equipment and wrestling mats —
Especially concerning in wrestling, where skin-to-skin contact is constant
Environmental Sources:
- Contaminated soil — Working in gardens or playing in dirt where fungal spores may be present
- Pet bedding — If you have an infected pet, their bedding contains spores
Why Ringworm Is So Contagious
Fungal spores are extremely resilient. They can survive on fabrics and surfaces for extended periods, sometimes for weeks. This is why ringworm spreads so easily and why it’s so common in:
- Schools and daycare centers (children in close contact)
- Gyms and fitness facilities (sweating, skin contact, shared equipment)
- Sports teams (wrestling, football, rugby—sports with skin-to-skin contact)
- Warm, humid climates (fungi thrive in heat and moisture)
Why Antifungal Treatment Takes Time
Now that you understand what causes ringworm, let’s explain why it doesn’t clear up immediately.
The reason ringworm doesn’t disappear overnight is because the infection involves a living organism that needs to be eliminated, and your skin needs time to heal afterward. When you apply an antifungal treatment, the medication works by interfering with the fungus’s ability to survive and grow. However, this process is gradual—not instant.
Why the process is slow:
- The fungus lives in your skin — The fungi aren’t just sitting on the surface. They’ve invaded the outer layer of your skin and are embedded there, feeding on keratin. Eliminating them takes time.
- Your skin needs to repair itself — Even after the fungus is addressed by antifungal medication, your skin still needs to replace the damaged cells and return to its normal state. This is a biological process that simply cannot be rushed. The outer layer of your skin is constantly shedding and regenerating, and healing happens as part of this natural cycle.
- Fungi are designed to persist — Fungi are particularly good at surviving in certain environments. They thrive in warm, moist conditions—which is why ringworm infections often persist longer in areas where you sweat, wear tight clothing, or experience friction. As long as conditions favor fungal growth, the infection will hang on.
- Antifungal medication works gradually — Antifungal treatments don’t kill the fungus instantly. Instead, they interfere with the fungus’s ability to grow and reproduce. Over days and weeks, the fungus population shrinks, but this is a gradual process, not an overnight cure.
How Long Does Ringworm Last? The Realistic Timeline
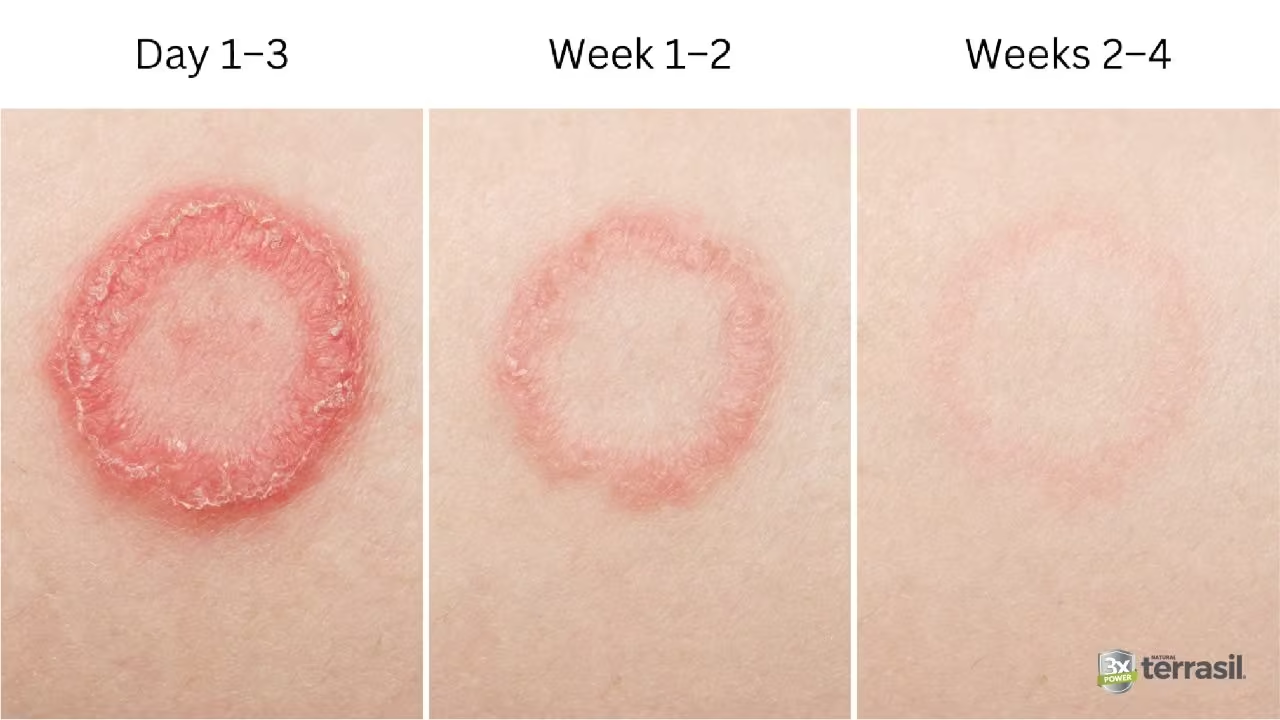
Let’s walk through what typically happens during treatment so you know what to expect at each stage.
Early Days (Days 1–3)
What you might notice:
In the first few days after starting antifungal treatment, you may notice some subtle improvements:
- Itching begins to decrease — The constant itch that’s been bothering you should start to feel less intense. This is usually the first sign that the treatment is working.
- Redness may appear less bright — The rash might not look quite as inflamed or angry.
- The rash stops expanding — One of the most reassuring early signs is when the rash stops growing outward, which means the fungus is no longer spreading.
Why these changes happen:
Antifungal ingredients begin affecting fungal cells early in treatment, which reduces irritation and stops the infection from spreading further. This is encouraging, and it’s natural to feel hopeful at this stage.
Important note: Early improvement does not mean the infection is gone. Many people make the mistake of stopping treatment too early because they think they’re cured. This is one of the biggest reasons ringworm lingers and comes back. The fungus is still present, even though symptoms are improving.
One to Two Weeks
What you might notice:
By week one to two, you should see more noticeable changes:
- The border of the rash begins to shrink — The outer edge of the rash becomes less distinct and starts moving inward. This is a sign that the infection is responding to treatment.
- Scaling and irritation improve — The flaky, irritated skin becomes smoother. The area might look and feel less uncomfortable.
- The center of the rash clears first — Often, the center of the circular rash clears before the edges, which is completely normal and expected.
Why this pattern happens:
The antifungal medication is systematically eliminating the fungus from the outside in. The infection doesn’t just disappear all at once—it gradually shrinks and fades. This is a healthy sign that your body is responding to treatment.
Several Weeks (Weeks 2–4+)
What you might notice:
As treatment continues:
- The rash typically continues to fade — The redness continues to diminish, and the skin begins to look more normal.
- The rash area becomes less raised — The texture of the skin smooths out and returns to normal.
- Overall improvement becomes more noticeable — The infected area increasingly blends in with surrounding skin.
Why treatment continues even when the rash is fading:
This is crucial to understand: you should continue using antifungal treatment for the full recommended duration on the product label, even after the rash looks like it’s gone.
When a rash looks clear, it can be tempting to stop treating it. However, fungal cells may still be present in the outer layer of your skin even though they’re no longer visible. Stopping treatment early allows these remaining fungal cells to regrow, and the infection returns. This is why the label directions matter so much.
Antifungal treatments typically continue for 2–4 weeks or longer, depending on the product and the severity of your infection.
Can Ringworm Go Away in 3 Days?
This is one of the most common questions people search online, and the honest answer is no.
While your itching and redness may begin to improve within 3 days of starting treatment, the infection itself requires much longer to fully resolve. Here’s why:
What 3 days of treatment accomplishes:
In just 3 days, antifungal medication can reduce inflammation and stop the fungus from spreading further. Your discomfort may decrease noticeably. This rapid improvement in symptoms can feel misleading—it makes you think the infection is almost over.
What 3 days cannot accomplish:
3 days is not enough time to eliminate all the fungal cells living on your skin. It’s also not enough time for your skin to fully repair the damage caused by the infection. The fungus has taken hold in the outer layer of your skin, and eliminating it completely requires consistent treatment over weeks.
The bottom line:
Expect improvement within days, but complete resolution usually requires consistent treatment over several weeks.
How Long Does Ringworm Last Without Treatment?

This is an important question because it shows why treatment matters.
Without antifungal medication, ringworm can persist for extended periods without treatment. Because the infection is caused by a living fungus, the rash will continue to slowly expand outward if the fungus remains active on your skin [1]. In some cases, untreated ringworm can spread to other areas of your body or to other people.
What happens without treatment:
- The fungus continues feeding on keratin in your skin
- The rash gradually expands in a circular pattern
- The infection can persist for months or even longer
- You risk spreading the infection to other people through direct contact or shared items
This is why antifungal treatment is so important. Without it, you’re essentially allowing the fungus to continue living and thriving on your skin.
Why some people delay treatment:
Some people hope ringworm will clear on its own or try home remedies first. While your immune system does fight fungal infections naturally, it’s often not powerful enough to eliminate the infection completely without antifungal medication. Treatment significantly accelerates the healing process and prevents the infection from spreading.
How Long Is Ringworm Contagious?
An important concern for many people is: how long can I spread this to others?
Ringworm spreads through contact with fungal spores. These microscopic spores can live on:
- Your infected skin
- Clothing and undergarments
- Towels and washcloths
- Bedding and blankets
- Shared surfaces like gym equipment or locker room floors
- Combs, hairbrushes, and personal grooming items
The contagious period:
Fungal spores can survive on fabrics and surfaces for a surprisingly long time—sometimes for weeks. This is why hygiene during treatment is so important. You can continue to spread ringworm even after you’ve started treatment, because:
- Fungal spores are still present on your skin during the early stages of treatment
- Spores remain on any items that have come into contact with the infected area
- These spores can transfer to other people if precautions aren’t taken
Practical steps to reduce spread:

- Wash towels, bedding, and clothing in hot water
- Don’t share personal items like combs, hairbrushes, or razors
- Keep the infected area covered when possible
- Wash your hands after touching the infected area
- Avoid close skin-to-skin contact with others, especially children
- Don’t share sports equipment or gym facilities
Transmission risk typically decreases after consistent treatment begins, though precautions are still important during treatment.
Why Your Ringworm Might Take Longer to Clear
Even with treatment, ringworm doesn’t always clear at the same speed for everyone. Some infections resolve quickly, while others linger. Several factors can slow down your healing.
Stopping Treatment Too Early
This is a common reason ringworm doesn’t clear.
One of the most common mistakes people make is stopping antifungal treatment as soon as the rash starts looking better. Even when the redness has mostly faded or the itching has nearly disappeared, the fungus is still present in the deeper layers of your skin.
The product label tells you how long to continue treatment for a reason. When you stop early:
- Remaining fungal cells regrow
- The infection returns, often within weeks
- You end up treating it again from the beginning
- The cycle repeats, and you feel frustrated
What to do instead:
Use your antifungal treatment for the full recommended duration, even if the rash is barely visible. Write down your start date and the end date on your calendar so you stay accountable.
Inconsistent Application
Antifungal treatments work gradually over time, and consistency is key.
If you skip applications, apply the treatment sporadically, or miss days, your progress will slow down. The antifungal ingredient needs to build up on your skin and maintain consistent contact with the fungus to eliminate it.
Why consistency matters:
Think of antifungal treatment like taking an antibiotic. If you take it every other day instead of every day as prescribed, the infection fights back. The same principle applies to topical antifungal creams. When you apply consistently, you maintain an environment where the fungus cannot survive.
Staying consistent:
- Apply the treatment at the same time each day (morning or night, whichever you prefer)
- Set a phone alarm or reminder
- Keep the product in a visible spot so you don’t forget
- Apply it right after you shower when your skin is clean and dry
Moisture and Friction
Fungi absolutely love warm, moist environments. This is why ringworm often appears in areas where you sweat, like:
- Between your toes (athlete’s foot)
- In your groin area
- Under your arms
- Under the breasts
- Anywhere skin rubs together
Why this slows healing:
If the infected area stays damp from sweat or moisture, the fungus has ideal conditions to continue growing even while you’re treating it. Tight, non-breathable clothing traps moisture and creates the perfect environment for fungi to thrive.
What to do about it:
- Keep the infected area clean and dry
- Change out of sweaty clothes as soon as possible
- Wear breathable fabrics like cotton instead of synthetics
- Avoid overly tight clothing during treatment
- Dry the area thoroughly after bathing or swimming
- Consider using antifungal powder in addition to cream if the area stays moist
Re-Exposure From Contaminated Items
Another reason ringworm returns is reinfection from contaminated clothing, towels, or bedding.
Ringworm spores can survive on fabrics for weeks. If you’ve treated the infection on your skin but continue sleeping on contaminated bedding or wearing contaminated clothing, you can continuously re-expose yourself to the fungus.
Preventing reinfection:
- Wash all towels, bedding, and clothing that came into contact with the infected area in hot water
- Wash these items separately from other laundry
- Dry in a hot dryer (the heat kills spores)
- Don’t reuse towels that touched the infected area
- Change your pillowcase and sheets more frequently
- Wash any items you’ve worn during treatment
If you’re dealing with repeated infections, read our guide on why ringworm keeps coming back and how to stop it.
The Quality of Your Treatment Product
Since ringworm treatment typically continues for several weeks, the overall formulation of the product you choose matters more than you might think.
Why product choice affects consistency:
A poorly formulated antifungal cream might:
- Feel greasy or heavy on your skin
- Stain your clothing
- Irritate your skin
- Feel uncomfortable to wear, making you less likely to apply it consistently
- Leave your skin feeling dry and tight
When a treatment feels uncomfortable, it’s harder to stay motivated to use it every single day for weeks. This is why dermatological products are designed with both active ingredients and supporting ingredients that work together.
For example, a well-formulated antifungal cream might combine:
- Clotrimazole 1% — a clinically recognized antifungal ingredient that targets the fungus
- Activated Minerals® technology — designed to support the skin environment during treatment
- Botanical ingredients commonly used to help soothe irritated skin
When your treatment feels pleasant to apply and soothes your skin, you’re much more likely to use it consistently, which directly impacts how quickly your infection clears.
Understanding Antifungal Ingredients

Most ringworm treatments work using one of several antifungal active pharmaceutical ingredients (APIs). Understanding how these work can help you choose an effective treatment.
Common antifungal ingredients include:
- Clotrimazole — works by interfering with the fungal cell membrane
- Terbinafine — disrupts the fungus’s ability to produce a protective wall
- Miconazole — similar mechanism to clotrimazole
- Tolnaftate — interferes with fungal growth
All of these are recognized as effective when used according to product directions [1][2].
How to choose:
If you want a detailed comparison of how these antifungal ingredients work and their specific strengths, we recommend reading our guide, Best Ringworm Cream – What Actually Works. This article breaks down each ingredient, how they differ, and what the clinical evidence says about their effectiveness.
The active ingredient is important, but remember that how the entire formula feels on your skin also matters. If you’re going to be applying a treatment multiple times daily for several weeks, the product needs to feel good enough that you’ll actually use it consistently.
Myth vs. Fact: Clearing Up Common Misconceptions
There’s a lot of misinformation about ringworm online. Let’s clear up what’s actually true.
Myth: “Ringworm is caused by worms”
Fact: Ringworm is caused entirely by fungi, not worms. The name is misleading—it comes from the circular, ring-like shape of the rash, not from what causes it. Dermatophyte fungi are tiny organisms that live on your skin. They’re completely different from parasitic worms and require completely different treatment. Antifungal creams are designed to target these fungi, while they would do nothing against a worm infection.
Myth: “Ringworm disappears overnight once you start treatment”
Fact: Symptom improvement may begin within several days, but the infection itself takes weeks to fully clear. Even when the rash looks like it’s almost gone, antifungal treatment should continue for the full recommended period. Many people see their rash fade after a week or two and assume they’re cured, only to have it return because they stopped treatment too early.
Myth: “Only children get ringworm”
Fact: Ringworm can affect people of any age—children, teenagers, adults, and older adults. While it is common in children (especially in schools and daycare settings), adults catch it regularly too. Athletes, gym members, and people in warm, moist climates experience it frequently. Age doesn’t make you immune.
Myth: “You should scratch ringworm to help it heal”
Fact: Scratching actually makes things worse. When you scratch the infected area, you:
- Spread fungal spores to other parts of your body
- Spread spores to other people through your fingernails
- Damage your skin barrier further, making infection worse
- Risk introducing bacteria that can cause a secondary bacterial infection
- Increase itching by irritating the area
Keep your nails trimmed and try to resist the urge to scratch. If itching is unbearable, ask a healthcare provider about options.
Myth: “You can treat ringworm with home remedies alone”
Fact: While some home remedies may provide temporary relief (like keeping the area dry or using tea tree oil), they are not typically strong enough to eliminate a fungal infection on their own. Antifungal medications are specifically formulated to target and kill the fungus. Home remedies might reduce symptoms, but they don’t address the root cause. Treatment with antifungal medication is the most effective approach.
Myth: “Once ringworm is treated, you can never get it again”
Fact: You can get ringworm more than once. Fungal infections don’t provide lasting immunity. Once you’ve had ringworm, you can catch it again from contaminated surfaces, other people, or animals. Good hygiene and avoiding exposure reduces your risk, but immunity doesn’t develop.
What Does Healing Look Like? How to Know Your Treatment Is Working
Knowing what progress looks like helps you stay motivated during treatment.
Signs that your treatment is working:
- Reduced itching — The constant itch becomes less intense and bothersome
- Fading redness — The rash is less bright red and more subtle
- Shrinking border — The outer edge of the rash moves inward rather than outward
- Cleared center — The middle of the circular rash clears first
- Smoother texture — The flaky, scaly appearance improves
- Less visible after a few weeks — By week 2–3, the rash should be noticeably less obvious
Signs that something might be wrong:
- The rash is expanding after 1 week of treatment — This suggests the fungus is still active, which might mean inconsistent application, reinfection from contaminated items, or the need for a different treatment approach
- Severe itching increases — While mild itching might decrease initially, severe itching that worsens might indicate a different condition
- Signs of a secondary infection — Pus, warmth, increased redness, or swelling might indicate bacteria have infected the area
If you’re not seeing improvement after 2–3 weeks of consistent treatment, or if the infection seems to be worsening, it’s worth discussing with a healthcare provider.
When Ringworm Appears to Come Back
Sometimes, after treatment seems to have cleared the infection, ringworm returns weeks or months later.
What’s actually happening:
In most cases, this isn’t the original infection returning—it’s reinfection from fungal spores that survived on your clothing, bedding, towels, or other items.
Why reinfection happens so often:
- You treated your skin successfully, but didn’t thoroughly wash contaminated fabrics
- Fungal spores survived on items in your environment
- Those spores came into contact with your skin again, starting a new infection
- You repeat the cycle of treating your skin without treating your environment
Preventing recurring ringworm:
- Wash all bedding, towels, and clothing in hot water
- Dry items in a hot dryer (heat kills spores)
- Don’t reuse items that touched the infected area
- Replace items like pillows or bath mats if possible
- Clean shared surfaces (bathroom counters, shower floors)
- Keep the previously infected area clean and dry to prevent reinfection
- Treat family members if they show signs of ringworm
If you’re experiencing recurring infections repeatedly, we recommend reading our detailed article Why Ringworm Keeps Coming Back (and How to Stop It for Good), which explains the most common causes of reinfection and specific prevention strategies.
Choosing the Right Antifungal Treatment
When selecting a ringworm treatment, you’re looking at two things: the active ingredient and the overall formula.
The active ingredient matters:
As mentioned earlier, common antifungal ingredients include clotrimazole, terbinafine, miconazole, and tolnaftate. These are all recognized for treating fungal skin infections when used according to product directions.
However, the active ingredient is only part of the equation.
The overall formula also matters:
Since you’ll be applying treatment daily for several weeks, consider:
- Does it feel comfortable on your skin? — Greasy formulas feel heavy; dry formulas might irritate. A balanced formula feels pleasant enough to use consistently.
- Will it stain clothing? — Some creams stain or discolor clothes, which makes them annoying to use regularly.
- Does it soothe irritated skin? — Ingredients like botanicals and minerals can reduce itching and irritation while the antifungal medication works.
- Does it moisturize? — Antifungal treatment can sometimes dry out skin. A formula that includes moisturizing ingredients supports your skin’s health during treatment.
Example of a well-formulated approach:
Terrasil® Ringworm Treatment combines clotrimazole 1% (a clinically recognized antifungal ingredient) with Activated Minerals® technology and botanicals selected for their soothing and moisturizing properties. This approach addresses both the fungal infection and your skin’s comfort, making consistent daily application feel sustainable over several weeks.
When treatment requires daily application for an extended period, choosing a product that’s designed with both efficacy and comfort in mind helps support your consistency—and consistency directly impacts how quickly your infection clears.

Ringworm Healing Timeline: Quick Reference Table
Stage | Timeframe | What to Expect |
|---|---|---|
Early treatment | Days 1 – 3 | Itching decreases, redness less intense, rash stops expanding |
Early improvement | Week 1 | Redness begins fading, border becomes less distinct |
Noticeable progress | Weeks 1 – 2 | Border shrinks inward, scaling improves, center clears |
Significant clearing | Weeks 2 – 4 | Rash continues fading, texture smooths, overall appearance improves |
Continued treatment | Weeks 3 – 6+ | Continue treatment per product label even if rash is mostly gone |
Full resolution | After treatment ends | Skin returns to normal; risk of reinfection decreases |
Frequently Asked Questions About Ringworm Cream
Conclusion
If you’re asking how long ringworm lasts, the realistic answer is that it requires patience. Fungal infections take time to resolve because they involve a living organism that must be eliminated, and your skin needs time to repair the damage.
Here’s what you need to remember:
- Symptom improvement begins within days, but complete healing takes weeks. Your itching and redness may decrease quickly, but the infection itself requires 2–4 weeks or longer to fully clear.
- Consistency matters more than anything else. Using your antifungal treatment every single day, exactly as directed, is the single most important factor in how quickly you heal.
- Don’t stop treatment early. Even when the rash looks mostly gone, continue using your antifungal medication for the full recommended duration. Stopping early is the #1 reason ringworm returns.
- Your environment matters. Wash contaminated fabrics, keep the infected area clean and dry, and avoid reinfection from your own clothing and bedding.
- A well-formulated treatment can help support consistency. When your antifungal product feels good on your skin and soothes irritation, you’re more likely to apply it consistently, which accelerates healing.
Understanding the realistic timeline helps you stay motivated and committed to treatment. Ringworm isn’t a quick fix, but with consistent antifungal treatment, you will see steady improvement week after week until the infection fully clears.
If you’re not seeing improvement after 3–4 weeks of consistent treatment, or if your infection seems to be worsening, reach out to a healthcare provider for guidance.
Disclaimer
This article is for informational and educational purposes only and is not intended to provide medical advice, diagnosis, or treatment recommendations. The information presented reflects general knowledge about fungal skin infections and over-the-counter antifungal treatments. Always read and carefully follow all product label directions before using any treatment product. If you have questions about your specific condition or whether a particular treatment is appropriate for you, consult a qualified healthcare provider. Do not use this article as a substitute for professional medical advice.
References:
- Centers for Disease Control and Prevention (CDC). Ringworm and Fungal Infections. Retrieved from https://www.cdc.gov/fungal/ringworm/index.html
- American Academy of Dermatology (AAD). Ringworm: Diagnosis and Treatment. Retrieved from https://www.aad.org/