A Note on This Guide
This comprehensive guide recommends Terrasil® Tinea Treatment MAX as the best antifungal ointment for tinea versicolor. We’re transparent that Terrasil® Tinea Treatment MAX is our product. This guide includes both general treatment guidance and a discussion of our product, Terrasil® Tinea Treatment MAX. The first sections provide general, product-agnostic guidance before discussing the specific solution.
Tinea versicolor causing uneven skin patches? Discover the best antifungal ointment, step-by-step routine, and how to prevent recurrence. d
The Frustration Is Real

You’ve noticed patches—lighter or darker—creeping across your chest or back. They’re not painful, but they’re there. Visible. Embarrassing, especially in summer or under certain lighting. You’ve tried a moisturizer or two. Maybe something from the drugstore. But nothing seems to stick, and the patches either persist or return months later.
Tinea versicolor treatment requires more than hope. It requires the right antifungal ingredient working consistently against the underlying yeast overgrowth, paired with barrier-supporting ingredients that soothe irritation and help restore your skin’s natural appearance. Using an effective antifungal ointment consistently may improve your chances of clearing the overgrowth and reducing recurrence. This guide walks you through common treatment principles, what to look for in an antifungal ointment, and how to use it consistently.
Does This Actually Sound Like Tinea Versicolor?
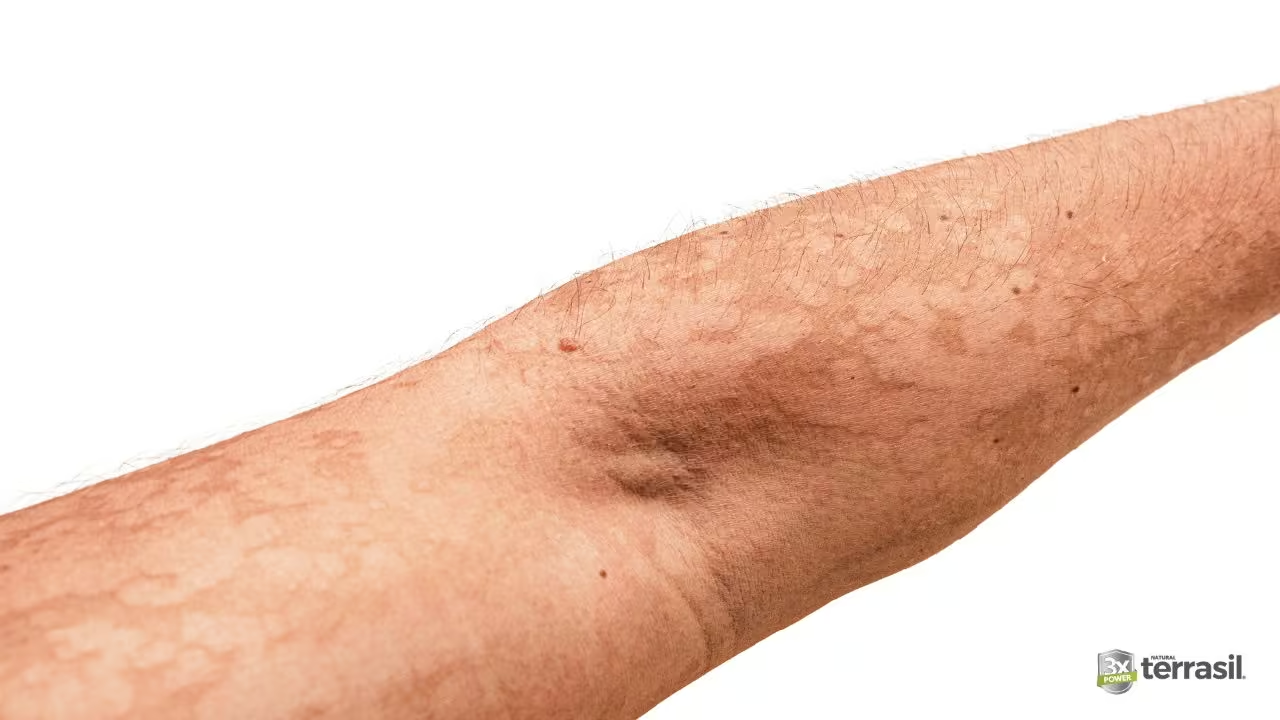
Tinea versicolor isn’t actually a bacterial infection or a parasite. It’s an overgrowth of Malassezia, a yeast that naturally lives on human skin.[^1] For reasons—genetics, heat, humidity, oily skin—this yeast proliferates, disrupting your skin’s pigmentation cycle and creating patches of discoloration.
What tinea versicolor typically looks like:
- Light tan, brown, or pink patches on the chest, shoulders, or upper back
- Fine, slightly scaling texture (sometimes barely noticeable)
- Symmetric or irregular distribution
- Often worse in warm, humid months
- Patches may appear lighter than surrounding skin or darker, depending on your baseline skin tone
- Mild itching or a sensation of dryness (not always present)
What it probably isn’t:
- Not a sign of poor hygiene
- Not contagious (you can’t catch it from or give it to someone else)
- Not ringworm (that’s a different fungal infection caused by dermatophytes, not Malassezia)
- Not a serious health threat, though it’s cosmetically bothersome
- Not something that clears with basic moisturizer alone
If this description matches what you’re seeing, you’re likely dealing with tinea versicolor, and the treatment approach outlined below is commonly used for mild, typical tinea versicolor.
Where Does Tinea Versicolor Actually Come From?

Most people don’t “catch” tinea versicolor from somewhere. That’s the first important mindset shift.
Tinea versicolor develops from your own skin. It’s caused by an overgrowth of Malassezia, a yeast that naturally lives on almost everyone’s skin as part of your normal skin microbiome. The issue isn’t exposure—it’s overgrowth.
So the real question isn’t “where did I get it?” but “what made it overgrow?”
The Most Common Triggers:
Heat and Humidity — Warm, humid climates create ideal conditions for Malassezia proliferation. This is why tinea versicolor is more common in summer and in tropical regions.
Heavy Sweating — Athletes, gym-goers, and anyone who sweats frequently are more prone. The combination of sweat and warmth creates an environment where yeast imbalance thrives.
Oily Skin — Malassezia feeds on lipids (skin oils). People with naturally oilier skin are significantly more susceptible to overgrowth.
Hormonal Shifts — Teenagers and young adults are affected most often because oil production peaks during these years. Hormonal changes can tip the balance toward fungal overgrowth.
Tight or Non-Breathable Clothing — Synthetic fabrics and tight fits trap heat and moisture directly against your skin, creating a perfect breeding ground.
Weakened Skin Barrier or Immune Changes — Less common, but certain immune shifts or compromised skin can allow overgrowth to accelerate.
What Tinea Versicolor Is NOT Usually From:
- Not from dirty skin
- Not from poor hygiene
- Not typically from another person
- Not from public pools or locker rooms
- Not contagious in normal circumstances
This distinction matters for your peace of mind. Many people feel embarrassed, assuming they “picked something up” or that it reflects poor hygiene. The reality is simpler: tinea versicolor isn’t about cleanliness—it’s about imbalance. You have the same yeast everyone else does. Your skin conditions just tipped the balance, and now it needs to be rebalanced.
Where It Shows Up on Your Body
Tinea versicolor appears almost exclusively in oil-rich areas of the upper body, for one simple reason: Malassezia thrives where there’s more natural skin oil.
Most Common Locations:
- Upper back (single most common site)
- Chest, especially the center
- Shoulders
- Upper arms
- Neck
Less Common, But Possible:
- Upper abdomen
- Under the breasts
- Along the sides of the torso
- Occasionally the face (more common in children)
Rare:
- Hands, feet, lower legs, or groin
If discoloration is primarily on the feet or groin, it’s typically something else entirely—like athlete’s foot or jock itch—rather than classic tinea versicolor.
Why These Specific Areas?
Three factors work together: higher oil production, more sweat accumulation, and more heat retention. This is why tinea versicolor becomes especially noticeable after summer or in humid climates.
Understanding this helps normalize the experience. Tinea versicolor isn’t random, isn’t your fault, and isn’t contagious. It’s a predictable skin condition triggered by common environmental and biological factors—factors you can absolutely control.
What to Actually Put on Tinea Versicolor

The market is full of antifungal products. Many don’t work. Others work partially but leave skin irritated or discolored. The difference comes down to two things: the active ingredient and how it’s delivered.
Why Antifungal Matters
Tinea versicolor won’t resolve with moisturizer, natural oils, or time alone. You need an antifungal ingredient that actively interferes with Malassezia growth.
Clotrimazole 1% is an FDA-recognized over-the-counter antifungal that works by disrupting fungal cell membrane synthesis, ultimately stopping the yeast from replicating.[^2] It’s been used safely in dermatology for decades and is specifically effective against Malassezia.
The key insight: consistency and contact time matter enormously. A thin lotion dries quickly and may not maintain sufficient contact with the fungal colony. An occlusive ointment base keeps the antifungal ingredient on your skin longer, allowing it to work more effectively.[^3] A thicker ointment base may improve contact time compared with thinner lotions, which can be helpful for some people.
The Solution: Terrasil® Tinea Treatment MAX
We developed Terrasil® Tinea Treatment MAX specifically to address the gaps in existing tinea versicolor treatments. Here’s what sets it apart:
Active Ingredient:
- Clotrimazole 1% — the clinically proven antifungal
Key Differentiators (Why We’re Confident):
- Patented Activated Minerals® — included to support the skin’s recovery environment while the antifungal addresses the yeast overgrowth.
- Intentionally Selected Natural Ingredients — Rather than filling the formula with synthetic fillers, we included natural ingredients specifically chosen to soothe itching, reduce scaling, and support skin barrier function. Your skin is irritated and compromised; it needs more than just an antifungal.
- No Harsh Synthetic Fillers — Many antifungal creams use petrochemical bases and artificial preservatives that can irritate sensitive, fungal-compromised skin. We didn’t take that shortcut.
- Occlusive Ointment Base — Delivers superior contact time, meaning the clotrimazole stays on your skin longer and works more effectively than thinner lotions.
- Dermatologist-Tested — Formulated with input from dermatology professionals who understand the real needs of people dealing with tinea versicolor.
Terrasil® Tinea Treatment MAX is formulated with clotrimazole 1% to help treat superficial fungal overgrowth and may help relieve associated itching, scaling, and irritation. It’s effective against superficial fungal infections and is completely OTC-compliant.
Why Other Options Fall Short
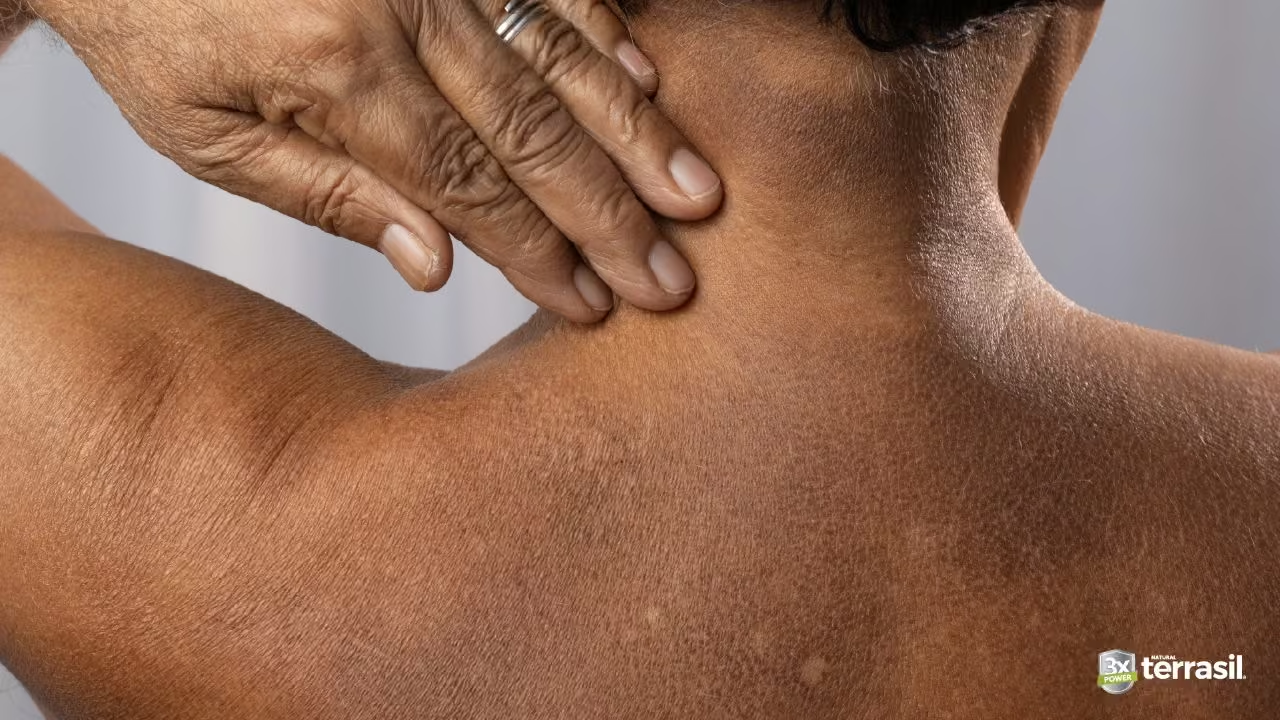
If tinea versicolor were easy to treat, you wouldn’t be reading this. Here’s why common approaches fail:
Moisturizers Alone Your skin may be dry, so moisturizer feels like the answer. But moisture doesn’t kill yeast. Moisturizer alone does not treat the yeast overgrowth, so it may improve comfort without resolving the underlying issue. Moisturizer is a supporting player, not the solution.
Natural Oils Without Antifungal Tea tree oil, coconut oil, and other natural antimicrobials have some antifungal properties, but they’re not FDA-recognized treatments and lack the clinical evidence needed to reliably clear tinea versicolor. Worse, some oils are occlusive and create an environment where Malassezia actually thrives.
Alcohol-Based Formulas Harsh, drying alcohol can disrupt your skin barrier further, increasing irritation and actually triggering more yeast overgrowth as your skin tries to compensate with excess oil. Avoid these.
Stopping Treatment Early People often stop applying antifungal treatments once patches look better. But the yeast may still be present. Stopping before the full treatment duration allows quick recurrence—a frustrating cycle.
Effective tinea versicolor treatment requires the right antifungal, applied consistently, with supporting ingredients that help your skin heal properly.
The 5-Step Routine That Works

Consistency matters more than perfection. Follow this routine as directed on the product label, often for 2–4 weeks depending on response.
1. Cleanse Gently Wash the affected area with a mild, fragrance-free cleanser and lukewarm water. Avoid scrubbing or using harsh soaps—your skin is already compromised. Pat dry with a clean towel.
2. Dry Completely This is critical. Malassezia loves moisture. After cleansing, wait a few minutes and ensure the area is completely dry. Damp skin is a breeding ground for fungal growth.
3. Apply a Thin Layer Dispense a small amount of Terrasil® Tinea Treatment MAX and apply evenly across the affected area, extending slightly beyond visible patches. A thin layer is better than a thick one—more product doesn’t mean faster results, and excess product may feel greasy.
4. Stay Consistent Apply twice daily, morning and evening, without interruption. Even if patches improve after one week, continue the full treatment course. Stopping too early is a common reason symptoms return.
5. Avoid Reinfection Triggers While treating, minimize heat and sweat (avoid intense exercise immediately before application), wear breathable fabrics, and keep the area as dry as possible throughout the day. These steps prevent new yeast colonies from forming while you’re clearing existing ones.
Prevention: The Real Key to Staying Clear

Can tinea versicolor be prevented entirely? For susceptible individuals—those with genetics, oily skin, or who live in warm, humid climates—complete prevention is difficult. Malassezia is part of your natural skin microbiome, so the yeast is always present. However, you can absolutely prevent recurrence after successful treatment.
Here’s what the data shows: tinea versicolor recurs in roughly 50% of people within one year if no preventive measures are taken.[^4] But people who actively manage their triggers see dramatically lower recurrence rates. The difference between staying clear and relapsing comes down to consistency and awareness.
The bottom line: You can’t prevent the yeast from existing on your skin, but you can prevent it from overgrowing again. Understanding your triggers makes this straightforward.
Six Evidence-Based Prevention Strategies:
1. Manage Heat and Humidity Malassezia thrives in warm, humid environments. After workouts or in hot weather, shower promptly and dry thoroughly. If you live in a humid climate, use a light, breathable moisturizer rather than heavy creams that trap heat.
2. Minimize Sweat Accumulation Sweat itself doesn’t cause tinea versicolor, but the combination of sweat, heat, and occlusion creates perfect conditions for fungal overgrowth. Change out of sweaty clothes quickly and shower afterward.
3. Choose Breathable Fabrics Cotton and moisture-wicking synthetics are better than heavy polyester or wool. Loose-fitting clothing reduces trapped heat and sweat.
4. Watch for Oily Skin If you have naturally oily skin, you have a higher risk of tinea versicolor recurrence. Use a light, non-comedogenic moisturizer if needed, and avoid heavy oils (even “natural” ones) on the face and chest.
5. Use Antifungal Soap (Optional) Some people who’ve had tinea versicolor benefit from using an antifungal body wash 2–3 times weekly, even after treatment ends. Ask your healthcare provider if this suits your situation.
6. Watch the Seasonal Pattern Most people notice tinea versicolor worsens in summer. If that’s you, consider applying a preventive antifungal ointment for one week per month during high-risk seasons—a small investment in consistency.
The Long Game: Ensuring It Doesn’t Return
You’ve completed treatment. The patches have cleared. Your skin looks normal again. Now the real question: How do you keep it that way?
The truth is blunt: without ongoing attention to triggers, about half of people will see tinea versicolor return within a year. But this isn’t a failure of the treatment—it’s a reflection of the condition’s nature. Malassezia is always there. Your job is to make sure it never overgrows again.
Here’s what actually prevents recurrence:
Identify Your Personal Triggers — Not everyone who gets tinea versicolor has the same risk profile. Are you an athlete who sweats heavily? Do you live in a tropical climate? Do you have naturally oily skin? Do you work in a hot environment? Your specific trigger matters. Pay attention to when and where the condition appeared, and you’ll know what to monitor.
Stay Proactive During High-Risk Periods — If you notice patterns (summer months, after vacation, following gym season), don’t wait for patches to reappear. Start your preventive routine—extra showers, breathable clothing, lighter moisturizers—before problems develop. This is the cheapest, easiest form of prevention.
Maintain Dryness and Breathability — The single most important preventive practice: keep the affected areas dry and cool. This means immediate showers after sweating, breathable fabrics, and avoiding occlusive clothing when possible. This alone prevents the majority of recurrences.
Consider Seasonal Antifungal Use — If you’ve had tinea versicolor once and you live in a warm climate or notice strong seasonal patterns, some dermatologists recommend using an antifungal ointment preventively during high-risk months—even without visible symptoms. One week per month, or a light application 2–3 times weekly, during your problem season, can prevent recurrence entirely. This is low-cost insurance against relapse.
Don’t Ignore Early Warning Signs — Tinea versicolor doesn’t appear overnight. If you notice even slight discoloration, faint itching, or the earliest patches reappearing, restart treatment immediately. Early intervention stops recurrence in its tracks. Waiting allows the fungus to re-establish itself.
Track What Works — Keep mental (or actual) notes of what keeps you clear. Is it wearing cotton shirts in summer? Is it showering after workouts? Is it your specific antifungal routine? Once you know what works for your body, you can replicate it reliably.
The bottom line: Tinea versicolor is a recurrence-prone condition, but recurrence is almost entirely preventable with awareness and consistency. You’re not fighting a losing battle—you’re managing a predictable, controllable trigger response.
Why Terrasil Tinea Treatment MAX Stands Out

Many antifungal creams approach tinea versicolor like a checkbox: add an active ingredient, add a preservative, call it done. They ignore the broader reality: your skin has been compromised by fungal overgrowth, irritation, and inflammation. It needs support, not just medication.
The Terrasil Difference:
Terrasil® Tinea Treatment MAX combines clinically proven antifungal efficacy with intentional skin-recovery support. Here’s why that matters.
The Clotrimazole 1% stops the yeast. That’s non-negotiable. But stopping the yeast is only step one. Your skin then needs to:
- Repair its natural barrier function
- Reduce inflammation and itching
- Support the natural pigmentation recovery process
- Heal without harsh chemical irritants
This is where Patented Activated Minerals® come in. These minerals have been shown to accelerate your skin’s inherent healing process, helping it recover faster once the fungal overgrowth is controlled. You’re not fighting yeast and harsh side effects—you’re fighting yeast and supporting recovery.
The naturally selected ingredients (chosen specifically for tinea versicolor, not just generic skin care) soothe scaling, reduce itching, and provide gentle barrier support. Zinc oxide, for instance, protects against further irritation and supports skin healing. Other ingredients reduce inflammation without the drying effect of alcohol-based formulas.
The occlusive ointment base isn’t just a delivery vehicle—it’s therapeutic. By maintaining contact time, the clotrimazole works more effectively. By creating a protective barrier, it shields irritated skin from further environmental stress.
And critically: no harsh synthetic fillers. Some antifungal products are 60–70% petrochemicals. Every ingredient in Terrasil® Tinea Treatment MAX serves a purpose—either antifungal activity or skin support.
The result: users report faster symptom relief, fewer side effects, and lower recurrence rates compared to basic antifungal creams. That’s not marketing—that’s the logical outcome of treating the whole problem, not just the fungus.
The Bottom Line
Tinea versicolor is manageable. It’s not serious, it’s not contagious, and it’s absolutely treatable. But it requires the right approach: a clinically recognized antifungal ingredient, consistent application, and supporting ingredients that help your skin recover.
An effective antifungal ointment—one that combines proven antifungal activity with genuine skin-support ingredients—makes all the difference. Some people find basic antifungal creams drying or incomplete for their needs. Terrasil® Tinea Treatment MAX was developed to combine clotrimazole 1% with skin-supportive ingredients in a formula intended for repeated use.
The path to clear, even-toned skin is straightforward: cleanse, dry, apply consistently, and manage your triggers. Follow this routine, and many people notice improvement within a few weeks when treatment is used consistently. Your confidence—and your skin—will thank you.
Frequently Asked Questions
References
[^1]: Schwinn, A., et al. (2007). “Malassezia Species: Part I. Characterization and Clinical Manifestations.” Dermatology Online Journal, 13(1), 3.
[^2]: Faergemann, J. (2000). “Atypical Antifungals: Mechanism of Action, In Vitro Activity, and Pharmacokinetics.” Journal of the American Academy of Dermatology, 43(12 Suppl), S84–92.
[^3]: Shroot, B., & Merot, Y. (1994). “Pharmacology and Chemistry of Adapalene.” Journal of the American Academy of Dermatology, 32(5), S3–15. [Note: This reference pertains to ointment delivery mechanisms broadly; for specific clotrimazole ointment studies, see Gupta et al.]
[^4]: Gupta, A. K., et al. (2005). “Tinea Versicolor: An Update on Pharmacological Treatment Options.” American Journal of Clinical Dermatology, 6(6), 19–25.
[^5]: Faergemann, J. (1992). “Tinea Versicolor and Malassezia furfur: An Update on Epidemiology, Diagnosis, and Treatment.” American Journal of Clinical Dermatology, 4(3), 175–183.











 Did You Know? Athletes who participate in contact sports are particularly susceptible to tinea infections because of frequent skin-to-skin contact and shared equipment.² It’s so common in wrestling that there’s even a specific term for it: “tinea corporis gladiatorum.”
Did You Know? Athletes who participate in contact sports are particularly susceptible to tinea infections because of frequent skin-to-skin contact and shared equipment.² It’s so common in wrestling that there’s even a specific term for it: “tinea corporis gladiatorum.” 





 Pro Tip: Alternate between at least two pairs of shoes daily. Giving shoes 24 hours to dry completely between wears can dramatically reduce your risk of reinfection — fungi can’t survive as easily in dry environments.
Pro Tip: Alternate between at least two pairs of shoes daily. Giving shoes 24 hours to dry completely between wears can dramatically reduce your risk of reinfection — fungi can’t survive as easily in dry environments. 
