Medically reviewed for informational accuracy | Educational content only
You touched something — a metal clasp, a new lotion, a cleaning product, a plant — and now your skin is red, itchy, and angry. That’s contact dermatitis: one of the most common skin reactions there is, and one of the most frequently misidentified. Here’s what it actually looks like, what causes it, how long it sticks around, and what may help your skin recover.
What is Contact Dermatitis?
Contact dermatitis is an inflammatory skin reaction triggered by direct contact with a substance that either irritates the skin or provokes an immune response. The word dermatitis simply means skin inflammation — and in this case, the cause is something external that touched the skin.[1]
It is among the most common skin conditions seen by dermatologists and primary care providers, affecting an estimated 15–20% of the general population at some point in their lives.[2] It accounts for the majority of occupational skin disease and is a frequent cause of chronic hand rashes.[3]
Contact dermatitis is not contagious. You cannot spread it to another person, and it does not travel from one part of your body to another on its own — though scratching can spread residual irritants or allergens to new skin areas.
Key distinction: it always starts where contact happened
Unlike conditions such as eczema or psoriasis that can appear anywhere regardless of exposure, contact dermatitis always begins at the site where skin met the triggering substance. Where the rash is tells you where to look for the cause.
The Two Main Types: Irritant vs. Allergic

Contact dermatitis comes in two distinct forms that share similar symptoms but have different underlying mechanisms. Understanding the difference matters because the cause — and therefore the prevention strategy — differs significantly between them.
Irritant Contact Dermatitis (ICD)
- Most common type — accounts for roughly 80% of cases[3]
- Caused by direct physical or chemical damage to the skin barrier
- No immune sensitization required — anyone can develop it
- Symptoms appear within minutes to hours of exposure
- Common triggers: soaps, detergents, solvents, frequent hand-washing, wet work
- Usually stays confined to the contact area
Allergic Contact Dermatitis (ACD)
- Less common but longer-lasting when it occurs
- Requires prior sensitization — the immune system must have “learned” to react to a specific allergen
- First exposure: no symptoms. Subsequent exposures: reaction[2]
- Symptoms appear 12–72 hours after re-exposure
- Common triggers: nickel, fragrance, poison ivy, latex, preservatives
- Rash may spread beyond the contact site
Why you can react to something you’ve used for years
People sometimes develop allergic contact dermatitis to products they’ve used without issue for months or years. This is because allergic sensitization can develop over time with repeated exposure — the immune system gradually builds a response. One day, it crosses a threshold and reacts. This pattern is especially common with preservatives in skincare, fragrance compounds, and metals like nickel.
What Contact Dermatitis Looks Like
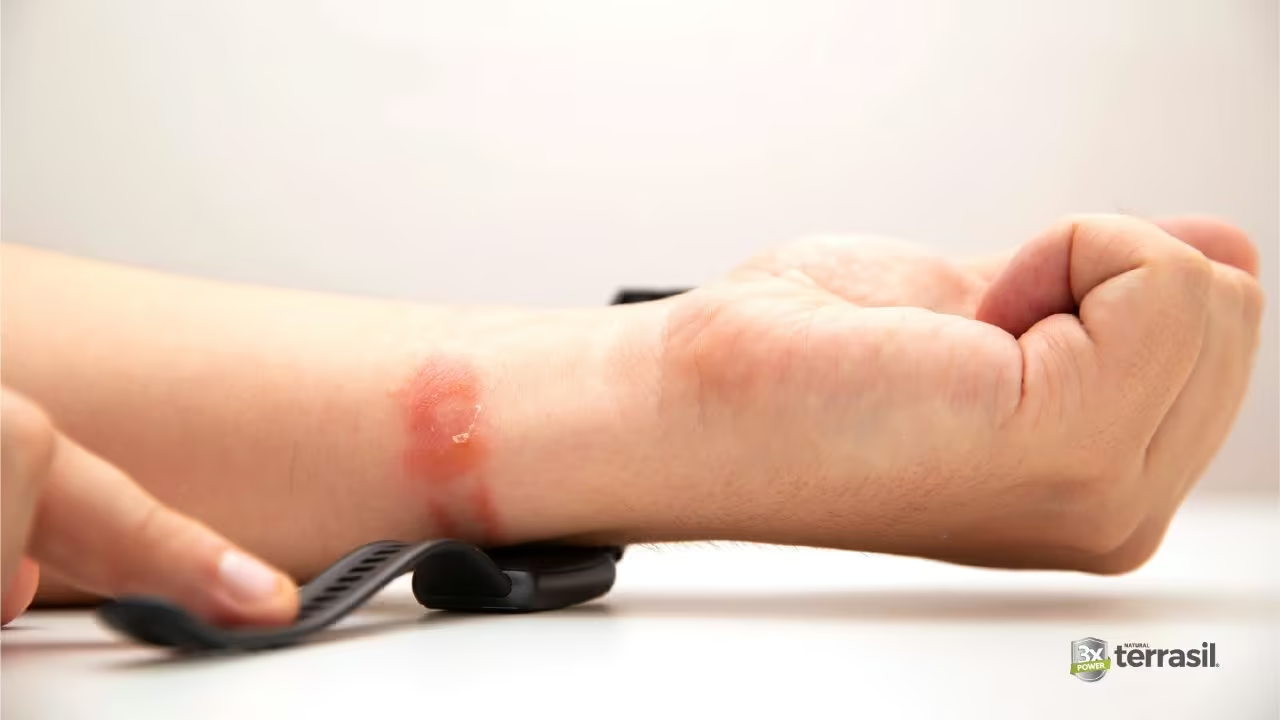
The appearance of contact dermatitis varies depending on how long the exposure has been happening, how severe the reaction is, and which type is involved. In general, the rash tends to be well-defined — appearing specifically where contact occurred rather than diffusely across the body.
Classic Visual Signs
- Redness: The affected skin typically appears red to deep pink, often with a clear boundary that corresponds to where the substance touched the skin — for example, the outline of a watchband or the shape of a belt buckle
- Swelling: The skin may look puffy or feel thickened; in more reactive cases, significant edema (fluid accumulation) can develop, particularly around the eyes or in loose skin areas
- Bumps and blisters: Small raised bumps (papules), fluid-filled blisters (vesicles), or larger blisters (bullae) may form — especially in allergic contact dermatitis from poison ivy or strong allergens[4]
- Oozing and crusting: Blisters may weep clear or slightly yellow fluid; once they rupture they often crust over
- Dry, flaky, or scaly skin: More common in chronic or subacute phases rather than the initial acute reaction
- Thickened skin (lichenification): With prolonged exposure or chronic scratching, the skin can become leathery and thickened over time[5]
The shape of the rash is a diagnostic clue
Because contact dermatitis follows the shape of what touched the skin, it often has unusually geometric, linear, or outline-shaped patterns that don’t appear in other skin conditions. A rectangular patch on the lower back may trace the outline of a jean button. A strip of rash on the wrist may follow the edge of a watchband. Earlobes, wrists, waistbands, and belt areas are classic locations for nickel-related allergic dermatitis.
Symptoms by Phase: Acute, Subacute, and Chronic
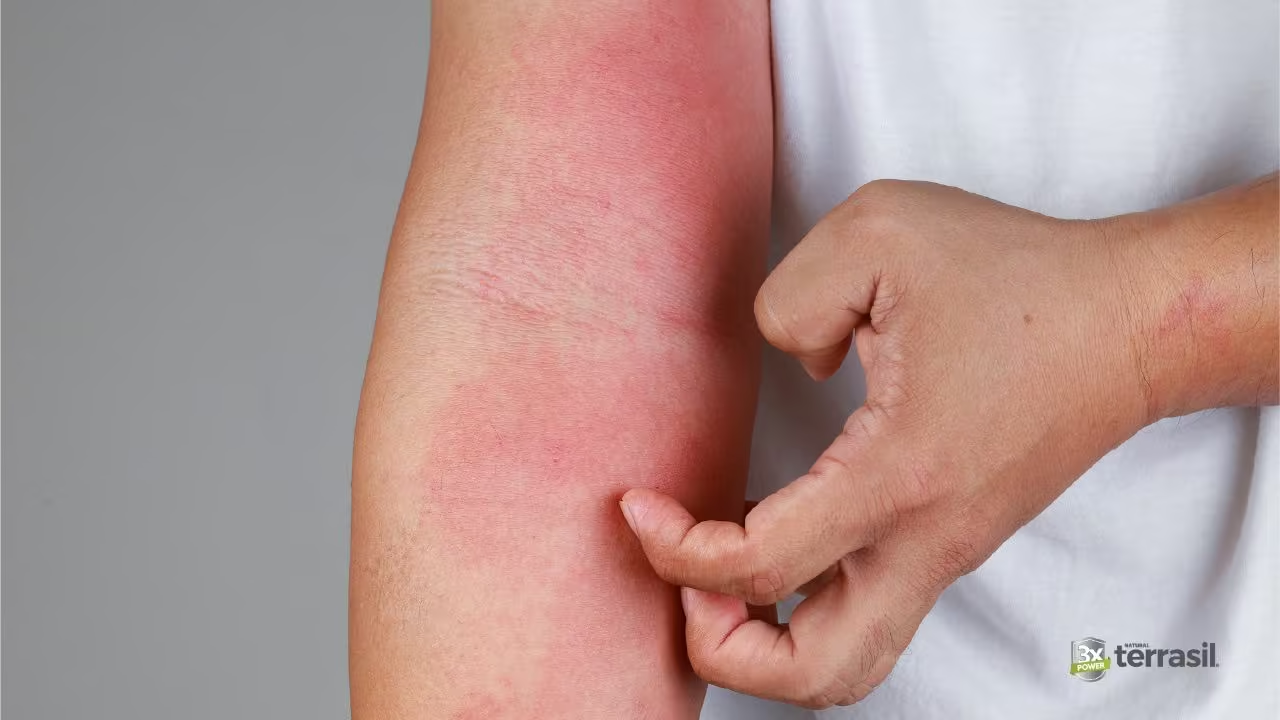
Contact dermatitis doesn’t look the same throughout its course. Clinicians classify it into three phases that each have a distinct appearance and symptom profile.[5] Recognizing which phase you’re in can help set realistic expectations for how the skin will change over time.
Hours to a few days after exposure. The skin responds rapidly and visibly — redness, swelling, and intense itching are the hallmarks. Blisters may form and rupture, leaving weeping, raw-looking skin. Burning and pain are also common in this phase, particularly with irritant dermatitis. This is when the reaction is at its most dramatic and uncomfortable.
- Subacute
Days to a couple of weeks in. The acute weeping begins to resolve. The skin starts to dry out, forming crusts and scales. Redness may persist but looks less raw and inflamed. Itching often remains significant. This is a transitional phase where the skin is actively working to repair the barrier.
- Chronic
Weeks to months with ongoing or repeated exposure. The skin becomes dry, cracked, and thickened (lichenified) from repeated inflammation and scratching. Scaling and hyperpigmentation (darkening of the affected area) may develop. This phase is common in occupational contact dermatitis — hands exposed daily to irritants often show this chronic pattern. The rash may be less visually dramatic but more persistent and uncomfortable.[6]
What Causes Contact Dermatitis? Common Triggers

The range of substances that can trigger contact dermatitis is enormous. Irritant and allergic triggers are different categories, though a single substance can sometimes act as both depending on the concentration and individual sensitivity.
Common Irritant Triggers
Cleansers & Soaps
Detergents, hand soaps, dish soap, shampoos — especially with frequent use or high-concentration formulas
Chemicals & Solvents
Cleaning products, paint, varnish, cement, gasoline, bleach, acids, and industrial solvents
Wet Work
Prolonged or repeated skin exposure to water — healthcare workers, food handlers, hairdressers, cleaners[3]
Physical Irritants
Fiberglass, sawdust, rough fabrics, friction, and abrasive materials
Low Humidity / Cold
Dry winter air strips skin moisture and weakens the barrier, increasing susceptibility to irritant reactions
Topical Products
Retinol, alpha-hydroxy acids, high-concentration actives in skincare when used too frequently or on compromised skin
Common Allergic Triggers
Metals
Nickel is the most common contact allergen worldwide — found in jewelry, belt buckles, jean buttons, watchbands, and medical devices[7]
Fragrances
Fragrance compounds in perfume, skincare, laundry products, and personal care items are among the top allergen categories
Preservatives
Methylisothiazolinone (MI), methylchloroisothiazolinone (MCI), parabens, and formaldehyde-releasing preservatives in cosmetics and personal care[8]
Plants
Poison ivy, poison oak, poison sumac — all contain urushiol, a potent contact allergen. Some tropical woods also cause reactions.
Rubber / Latex
Latex gloves, elastic waistbands, rubber-containing products — particularly relevant in healthcare settings
Hair Dye / PPD
Para-phenylenediamine (PPD) in permanent hair dyes is a frequent cause of scalp, neck, and earlobe allergic reactions
Adhesives
Medical adhesive tapes, bandage adhesives, sticker residue — particularly relevant for prolonged skin contact
Topical Medications
Neomycin (in antibiotic ointments), benzocaine, bacitracin — can cause allergic reactions with repeated application[9]
Where It Commonly Appears on the Body
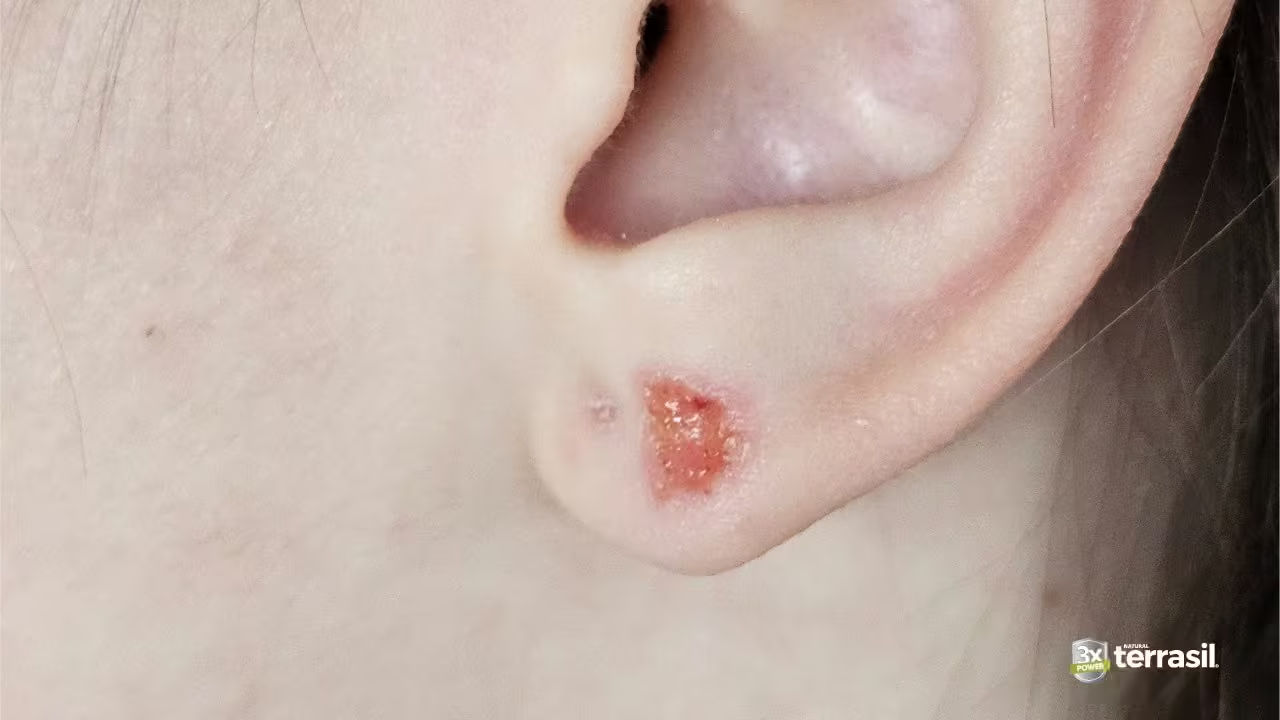
The location of contact dermatitis typically maps directly to the triggering substance and how it came into contact with the skin. Recognizing common location-trigger pairs can help identify what’s causing a reaction.
Body Location | Common Triggers | Notes |
|---|---|---|
Hands and fingers | Soaps, detergents, solvents, latex gloves, frequent hand-washing | Most common site overall; hands are affected in approximately 4 out of 5 cases of occupational contact dermatitis[6] |
Wrists | Watchband (nickel, rubber, leather), bracelets | Linear or band-shaped rash pattern that mirrors the band width and fit |
Earlobes and ear piercings | Nickel in jewelry — earrings, posts, clasps | Earlobes are one of the most classic locations for nickel allergy; reaction often begins at the piercing site |
Neck | Necklace metals, fragrance (applied to neck), hair dye[7] | Fragrance-related reactions often create a diffuse pattern; jewelry reactions follow the chain or clasp outline |
Waistband and abdomen | Jean buttons, belt buckles, waistband elastic — often nickel or rubber | Rash appears in the shape of the fastener; round or oval patches at the navel level are characteristic |
Lower legs and feet | Shoe materials (leather, rubber, adhesives), topical products applied to the legs | Shoe contact dermatitis may follow the outline of straps, insoles, or rubber soles |
Arms and legs (diffuse) | Poison ivy, poison oak — urushiol deposited on skin by contact or airborne spread | Linear streaks are characteristic — corresponding to where the plant leaf brushed the skin |
Genital / groin area | Latex condoms, spermicides, detergents, scented personal care products | The skin in this area is thin and highly sensitive; reactions may be more pronounced and longer-lasting[10] |
How Long Does Contact Dermatitis Last?
This is the question most people ask first — and the honest answer is that it depends significantly on the type of dermatitis, how quickly the trigger is identified and removed, how severe the reaction is, and what care is given to the skin during recovery.
Mild irritant: Days 1–7
Mild irritant contact dermatitis often begins clearing within a few days once the irritating substance is removed. Skin may remain slightly red or dry for up to a week but should progressively improve with gentle care.
Moderate irritant: 1–2 weeks
More significant irritant reactions may take one to two weeks to resolve. Cracking, scaling, and persistent redness are common. Barrier repair is the priority during this phase.
Allergic contact dermatitis: 2–4 weeks
Allergic reactions typically last longer than irritant reactions — commonly 2 to 4 weeks even after the allergen is fully removed.[11] This is because the immune response continues after allergen removal. The skin needs time to work through the inflammatory cycle.
Untreated or ongoing exposure: 4–8+ weeks
If the trigger is not identified and removed, or if exposure continues, contact dermatitis can persist for months and transition into a chronic pattern with thickened, cracked, or hyperpigmented skin.[12]
Chronic occupational dermatitis: Ongoing
In occupational settings where avoidance is difficult, chronic contact dermatitis may persist indefinitely without intervention. Barrier protection and workplace modifications are the primary management tools in these situations.
The key variable: removing the trigger
Nothing speeds recovery from contact dermatitis as reliably as stopping contact with whatever caused it. Without that step, even the best skincare routine is working against an ongoing source of inflammation. Identifying and eliminating the trigger is the single most impactful action.
Contact Dermatitis vs. Other Skin Conditions
Contact dermatitis is frequently confused with other inflammatory skin conditions that produce similar redness, itching, and rash patterns. The distinctions below can help clarify what’s happening — though a healthcare provider is the appropriate source for an actual diagnosis.
Condition | Typical Appearance | Key Distinguishing Features |
|---|---|---|
Contact dermatitis | Red, itchy, sometimes blistered; well-defined borders | Begins at the exact site of contact; clear link to an exposure; not present on unexposed skin |
Atopic dermatitis (eczema) | Red, dry, intensely itchy; often in skin folds | Chronic and recurring; appears without a specific external trigger; often starts in childhood; associated with asthma and hay fever[13] |
Psoriasis | Thick, silvery scales on raised red plaques | Autoimmune condition; plaques have a distinctive silvery scale; commonly affects elbows, knees, scalp; not triggered by external contact |
Ringworm (tinea corporis) | Ring-shaped rash with raised, scaly border and clearer center | Fungal infection; characteristic ring pattern; spreads outward; no clear link to a single contact event[14] |
Hives (urticaria) | Raised welts that appear and disappear within hours | Wheals resolve within 24 hours and move around the body; often triggered by food, medication, or systemic allergens rather than skin contact |
Candidal rash (yeast) | Bright red rash in skin folds; satellite pustules at edges | Favors warm, moist areas; satellite lesion pattern is characteristic; not linked to a specific contact exposure[15] |
What May Help Skin Recover
Managing contact dermatitis involves two parallel goals: reducing ongoing inflammation and irritation, and supporting the skin’s barrier as it repairs. The following approaches are commonly used — always in conjunction with removing the triggering substance.
Remove and Rinse First
If contact has just occurred with a known irritant or allergen, washing the affected area with mild soap and cool water as soon as possible may help reduce the severity of the reaction by removing residual substance from the skin surface.[11] This is particularly relevant with poison ivy — urushiol can continue to provoke a reaction if left on the skin.
Cool Compresses
Applying a clean, cool, damp cloth to the affected area may help calm acute inflammation, reduce itch intensity, and provide comfort during the most uncomfortable early phase. Avoid hot water, which tends to worsen inflammation and itching.
Barrier-Supporting Ingredients
The skin’s barrier function — its ability to retain moisture and block external irritants — is typically compromised in contact dermatitis. Ingredients such as shea butter, glycerin, and botanical oils may help support barrier recovery by reducing moisture loss and soothing inflamed tissue. Gentle, fragrance-free formulations are preferred during recovery, since fragrance is itself a common allergen that can worsen an already reactive skin environment.[8]
Avoiding Scratching
Scratching provides temporary itch relief but worsens the inflammation cycle — it further damages the skin barrier, opens the door to secondary infection, and can spread residual irritants or allergens to nearby skin. Keeping nails short and applying cool compresses when itch is intense may help break the scratch cycle.
Topical Corticosteroids
Over-the-counter hydrocortisone cream is commonly used to reduce inflammation and itch in mild to moderate contact dermatitis. Stronger prescription-strength topical corticosteroids may be recommended by a healthcare provider for more significant reactions. Long-term or high-strength corticosteroid use should be guided by a provider due to potential skin-thinning effects.[16]
Antihistamines
Oral antihistamines are sometimes used to help manage itching, though they address the itch symptom rather than the underlying inflammation. Sedating antihistamines may be particularly useful at night when itching can interfere with sleep.
Try Terrasil® Skin Repair Ointment

When skin is irritated, broken down, or recovering from a contact reaction, the barrier support and soothing properties of a product matter significantly. Terrasil® products are formulated with Activated Minerals® — a proprietary mineral delivery system — alongside botanical and skin-supportive ingredients.
For irritated, compromised, or inflamed skin
Terrasil® Anti-Bacterial Skin Repair
Terrasil Anti-Bacterial Skin Repair is formulated to support skin that has become inflamed, irritated, or compromised — which is often the condition of skin affected by contact dermatitis, particularly during the subacute and recovery phases. The formula includes Activated Minerals® along with beeswax, jojoba oil, and other botanical ingredients that may help soothe irritated tissue and support the skin’s recovery process.
Its ointment base provides a longer-lasting layer of skin contact and may help protect the skin surface while it heals — particularly useful when the affected area is still raw, cracked, or prone to friction.
When fungal overgrowth is a secondary concern
Terrasil® Antifungal Treatment MAX
Prolonged contact dermatitis — particularly in warm, moist areas like the groin, skin folds, or under occlusive bandaging — can compromise the skin barrier enough to allow secondary fungal overgrowth (candidal or tinea) to take hold.[15] If a rash is not improving as expected, or has characteristics suggesting fungal involvement alongside contact irritation (satellite lesions, moist maceration), Terrasil Antifungal Treatment MAX contains clotrimazole 1% USP as its active ingredient — a well-established antifungal agent — formulated with Activated Minerals® for enhanced delivery.
Patch testing: finding your specific allergen
If allergic contact dermatitis is suspected but the allergen is unclear, a dermatologist can perform patch testing — small amounts of common allergens are applied to the skin under adhesive patches for 48 hours, then evaluated for reactions. This is the gold standard for identifying which specific substance is triggering an allergic response.[17] It’s particularly valuable for people with recurrent, unexplained rashes or chronic dermatitis.
Prevention Tips
Once a contact dermatitis trigger is identified, the most effective prevention strategy is avoidance. Beyond that, several practices can reduce the likelihood of reactions and protect skin barrier integrity.
Identifying and Avoiding Your Triggers
- Read product ingredient labels carefully — particularly for fragrances, preservatives, and potential allergens
- Switch to fragrance-free, dye-free personal care and household products when possible
- Choose nickel-free jewelry or coat metal surfaces (e.g., belt buckles) with a clear barrier film or nail polish to reduce skin contact
- Learn to identify poison ivy, poison oak, and poison sumac in your local area
Protecting the Skin Barrier
- Apply a fragrance-free moisturizer or barrier cream after hand-washing and bathing to help replace moisture lost through cleansing
- Wear gloves when working with cleaning products, detergents, solvents, or other known irritants — both waterproof and cotton gloves may be appropriate depending on the task
- Avoid prolonged contact with water, especially combined with soaps or cleansers, without barrier protection
- Pat skin dry rather than rubbing after washing; rubbing generates friction that weakens the barrier over time
In Occupational Settings
- Use appropriate personal protective equipment (PPE) for the specific substances involved
- Apply barrier creams before exposure and moisturize after — not as a substitute for PPE but as a complement to it
- Report persistent skin reactions; occupational contact dermatitis is a recognized occupational disease with workplace protections in many jurisdictions[6]
Introducing New Products Carefully
- When trying a new skincare, fragrance, or personal care product, do a small patch test on the inner arm for 24–48 hours before full use
- Introduce one new product at a time so that if a reaction occurs, the cause is easy to identify
Frequently Asked Questions
The Bottom Line
Contact dermatitis is one of the most common skin reactions people experience — and one of the most manageable once the cause is identified. It begins where skin meets its trigger: an irritant that damages the skin barrier directly, or an allergen that the immune system has learned to react against. The rash it produces is typically well-defined, corresponds to the contact site, and progresses through distinct phases from acute to subacute to chronic depending on how the situation is handled.
How long it lasts depends almost entirely on two things: removing the trigger, and supporting the skin’s barrier as it repairs. Mild irritant reactions may clear in days. Allergic reactions can take weeks even after the allergen is gone. Chronic cases — particularly from occupational exposure — may persist without deliberate management.
Terrasil® Anti-Bacterial Skin Repair may offer supportive care for skin in the recovery phase — helping to soothe irritated tissue and support the barrier. When a secondary fungal concern is present alongside contact irritation, Terrasil® Antifungal Treatment MAX (clotrimazole 1% USP with Activated Minerals®) addresses that layer directly.
When in doubt about what’s causing a persistent rash, or when symptoms are severe, spreading, or not improving, a healthcare provider is the right next step — and patch testing can provide clarity when the allergen is unknown.
References
- Cleveland Clinic. Contact Dermatitis. Updated 2023. https://my.clevelandclinic.org/health/diseases/6173-contact-dermatitis
- Mowitz M, Svedman C. Allergic contact dermatitis revisited: A comprehensive review. JAAD Reviews. 2025. https://www.jaadreviews.org
- Langan SM, Irvine AD, Bhutani T. Irritant contact dermatitis — a review. Curr Dermatol Rep. 2022. https://pmc.ncbi.nlm.nih.gov/articles/PMC8989112/
- Litchman G, Nair PA, Atwater AR, Bhutta BS. Contact Dermatitis. In: StatPearls [Internet]. Updated 2023. https://www.ncbi.nlm.nih.gov/books/NBK459230/
- Usatine RP, Riojas M. Diagnosis and management of contact dermatitis. Am Fam Physician. 2010;82(3):249–255. https://www.aafp.org/pubs/afp/issues/2010/0801/p249.html
- Mälkönen T, et al. Occupational contact dermatitis. Best Pract Res Clin Dermatol. 2020. See also: DermNet NZ. Hand dermatitis. https://dermnetnz.org/topics/hand-dermatitis
- Brar KS. A review of contact dermatitis. Ann Allergy Asthma Immunol. 2021;126(1):32–39. https://www.annallergy.org/article/S1081-1206(20)31080-2/fulltext
- Johansen JD, et al. Novel insights into contact dermatitis. J Allergy Clin Immunol. 2022;149(4):1168–1180. https://www.jacionline.org
- American Academy of Dermatology Association. Contact dermatitis: Overview. https://www.aad.org/public/diseases/a-z/contact-dermatitis-overview
- Spire Healthcare. Contact Dermatitis. Updated 2023. https://www.spirehealthcare.com/conditions/contact-dermatitis/
- Mayo Clinic. Contact dermatitis — Diagnosis and treatment. Updated 2024. https://www.mayoclinic.org/diseases-conditions/contact-dermatitis/diagnosis-treatment/drc-20352745
- Expert Dermatology. How Long Does Contact Dermatitis Last? 2025. https://www.expertdermatology.com/how-long-does-contact-dermatitis-last/
- National Eczema Association. Atopic Dermatitis vs. Contact Dermatitis. https://nationaleczema.org/eczema/types-of-eczema/contact-dermatitis/
- American Academy of Dermatology Association. Ringworm: Overview. https://www.aad.org/public/diseases/a-z/ringworm-overview
- DermNet NZ. Candidal intertrigo. Updated 2023. https://dermnetnz.org/topics/candidal-intertrigo
- MedicalNewsToday. Contact dermatitis rash: Pictures, treatment, and more. Updated 2025. https://www.medicalnewstoday.com/articles/contact-dermatitis-rash
- Fonacier L, Bernstein DI, Pacheco K, et al. Contact Dermatitis: A Practice Parameter Update 2015. J Allergy Clin Immunol Pract. 2015;3(3 Suppl):S1–S39. https://www.jaci-inpractice.org
Disclaimer: This article is intended for informational and educational purposes only and does not constitute medical advice. Always read and follow product label directions. If you are uncertain about a skin condition or the appropriate care approach for your situation, consult a qualified healthcare professional.








